Do you worry about what is going to kill you? Heart disease, cancer, a car accident? Most of us worry about things we can't control, like war, terrorism, the tragic earthquake that just occurred in Haiti. But what really threatens humanity? A few years ago, Professor Vaclav Smil tried to calculate the probability of sudden disasters large enough to change history. He called these, "massively fatal discontinuities," meaning that they could kill up to 100 million people in the next 50 years. He looked at the odds of another world war, of a massive volcanic eruption, even of an asteroid hitting the Earth. But he placed the likelihood of one such event above all others at close to 100 percent, and that is a severe flu pandemic. Now, you might think of flu as just a really bad cold, but it can be a death sentence. Every year, 36,000 people in the United States die of seasonal flu. In the developing world, the data is much sketchier but the death toll is almost certainly higher. You know, the problem is if this virus occasionally mutates so dramatically, it essentially is a new virus and then we get a pandemic.
Da li brinete o tome šta će vas ubiti? Srčana bolest, rak, ili saobraćajna nesreća? Većina nas se brineo stvarima koje su van naše kontrole kao što su rat, terorizam, ili tragični zemljotres koji se desio na Haitiju. Međutim, šta zapravo preti čovečanstvu? Pre nekoliko godina, profesor Vaclav Smil je pokušao da izračuna verovatnoću iznenadnih katastrofa dovoljno velikih da promene istoriju. Nazvao ih je ''masovnim pomorima,'' što bi značilo da mogu ubiti do sto miliona ljudi u narednih pedeset godina. Razmatrao je mogućnosti za još jedan svetsti rat, za ogromnu vulkansku erupciju, čak i za udar asteroida u Zemlju. Verovatnoću za ozbiljnu pandemiju gripa je stavio blizu sto odsto, što je iznad do sada svih nabrojanih katastrofa. Sada, možete razmišljati o gripu kao o stvarno lošoj prehladi. A takodje može biti i smrtna presuda. Svake godine, 36 hiljada ljudi u Sjedinjenim Američkim Državama umre od sezonskog gripa. U svetu koji se razvija, podaci su mnogo šarolikiji ali smrtna stopa je skoro sigurno viša. Znate, problem je kada ovaj virus povremeno mutira toliko dramatično, da je u suštini novi virus pa nas onda zahvati pandemija.
In 1918, a new virus appeared that killed some 50 to 100 million people. It spread like wildfire and some died within hours of developing symptoms. Are we safer today? Well, we seem to have dodged the deadly pandemic this year that most of us feared, but this threat could reappear at any time. The good news is that we're at a moment in time when science, technology, globalization is converging to create an unprecedented possibility: the possibility to make history by preventing infectious diseases that still account for one-fifth of all deaths and countless misery on Earth. We can do this. We're already preventing millions of deaths with existing vaccines, and if we get these to more people, we can certainly save more lives. But with new or better vaccines for malaria, TB, HIV, pneumonia, diarrhea, flu, we could end suffering that has been on the Earth since the beginning of time.
Novi virus koji se pojavio 1918. godine ubio je oko pedeset do sto miliona ljudi. Širio se kao vatra neki su umirali i nekoliko sati nakon pojava simptoma. Jesmo li sigurniji danas? Pa, izgleda da smo ove godine izbegli smrtnu pandemiju koje se većina od nas plašila, međutim, ova pretnja se može opet pojaviti bilo kada. Dobre vesti su da smo u vremenu kada nauka, tehnologija, globalizacija teže ka istom praveći jedinstvenu mogućnost: mogućnost stvaranja istorije sprečavanjem zaraznih bolesti koje još uvek obuhvataju jednu petinu svih smrtnih slučajeva i bezbrojnih beda na Zemlji. Možemo to uraditi. Već sprečavamo milione smrtnih slučajeva sa postojećim vakcinama, i ako ih dostavimo do više ljudi, sigurno možemo spasiti više života. Sa novim ili boljim vakcinama od malarije, TB-a, HIV-a, zapaljenja pluća, dijareje, gripa, mogli bismo privesti kraju patnji koja je bila prisutna na Zemlji od početka vremena.
So, I'm here to trumpet vaccines for you. But first, I have to explain why they're important because vaccines, the power of them, is really like a whisper. When they work, they can make history, but after a while you can barely hear them. Now, some of us are old enough to have a small, circular scar on our arms from an inoculation we received as children. But when was the last time you worried about smallpox, a disease that killed half a billion people last century and no longer is with us? Or polio? How many of you remember the iron lung? We don't see scenes like this anymore because of vaccines.
Ovde sam da vam razglasim o vakcinama. Prvo, moram objasniti zašto su one važe jer vakcine, njihova moć, je zapravo kao šapat. Kada rade, mogu stvarati istoriju, dok posle izvesnog vremena jedva da možete da ih čujete. Sada, neki od nas su dovoljno stari da imaju mali, kružni ožiljak na rukama od vakcinisanja koje smo primili kao deca. A kada ste se zadnji put zabrinuli o malim boginjama, bolesti koja je prošlog veka ubila pola milijarde ljudi, a koja više nije sa nama? Ili dečije paralize? Koliko vas pamti gvozdena pluća? Više ne vidimo takve situacije zbog vakcina.
Now, it's interesting because there are 30-odd diseases that can be treated with vaccines now, but we're still threatened by things like HIV and flu. Why is that? Well, here's the dirty little secret. Until recently, we haven't had to know exactly how a vaccine worked. We knew they worked through old-fashioned trial and error. You took a pathogen, you modified it, you injected it into a person or an animal and you saw what happened. This worked well for most pathogens, somewhat well for crafty bugs like flu, but not at all for HIV, for which humans have no natural immunity.
Sada, zanimljivo je pošto postoji tridesetak bolesti koje možemo tretirati vakcinama, a još uvek smo ugroženi stvarima kao što su HIV i grip. Zbog čega? Evo u čemu je tajna. Donedavno, mi nismo tačno znali kako su radile vakcine. Znali smo da su radile preko staromodnih ispitivanja. Uzmete patogen, izmenite ga, ubrizgate ga u osobu ili životinju i gledate šta će se dogoditi. Ovo je dobro funkcionizalo za većinu patogena, ali manje za lukave bube kao što je grip, ali nikako nije za HIV, za koji ljudi nemaju prirodni imunitet.
So let's explore how vaccines work. They basically create a cache of weapons for your immune system which you can deploy when needed. Now, when you get a viral infection, what normally happens is it takes days or weeks for your body to fight back at full strength, and that might be too late. When you're pre-immunized, what happens is you have forces in your body pre-trained to recognize and defeat specific foes. So that's really how vaccines work. Now, let's take a look at a video that we're debuting at TED, for the first time, on how an effective HIV vaccine might work.
Istražimo kako vakcine rade. One prvenstveno naprave sklonište oružja za vaš imuni sistem koji možete iskoristiti kada je potrebno. Sada, kada dobijete virusnu infekciju, ono što se obično dešava je da su potrebni dani ili nedelje za vaše telo da odreaguje punom snagom, što može biti prekasno. Kada ste vakcinisani, dešava se to da imate snage u svom telu istrenirane tako da prepoznaju i poraze određene uljeze. Tako zapravo rade vakcine. Pogledajmo sada snimak po prvi put na TED-u o tome kako efektivne HIV vakcine mogu raditi.
(Music)
(Muzika)
Narrator: A vaccine trains the body in advance how to recognize and neutralize a specific invader. After HIV penetrates the body's mucosal barriers, it infects immune cells to replicate. The invader draws the attention of the immune system's front-line troops. Dendritic cells, or macrophages, capture the virus and display pieces of it. Memory cells generated by the HIV vaccine are activated when they learn HIV is present from the front-line troops. These memory cells immediately deploy the exact weapons needed. Memory B cells turn into plasma cells, which produce wave after wave of the specific antibodies that latch onto HIV to prevent it from infecting cells, while squadrons of killer T cells seek out and destroy cells that are already HIV infected. The virus is defeated. Without a vaccine, these responses would have taken more than a week. By that time, the battle against HIV would already have been lost.
Pripovedač: vakcina trenira telo unapred kako da prepozna i neutrališe određenog napadača. Nakon što HIV probije barijere sluzokože tela, on zarazi imune ćelije za obnovu. Napadač privlači pažnju prve linije fronta vojnika imunog sistema. Dendritske ćelije, ili makrofage, hvataju virus i prikazuju njegove deliće. Memorijske ćelije generisane HIV vakcinom se aktiviraju kada saznaju za prisustvo HIV-a od strane vojnika iz prve linije fronta. Ove memorijske ćelije odmah isporuče oružje koje je potrebno. Memorijske B ćelije se pretvore u plazmocite, koji proizvode talas za talasom određenih antitela koji se pričvršćuju na HIV i onemogućuju mu inficiranje ćelija, dok eskadrila ubijačkih T ćelija traži i uništava ćelije koje su već zaražene HIV-om. Virus je poražen. Bez vakcine, ovakva reagovanja bi trajala više od nedelju dana. Za to vreme, bitka protiv HIV-a bi već bila izgubljena.
Seth Berkley: Really cool video, isn't it? The antibodies you just saw in this video, in action, are the ones that make most vaccines work. So the real question then is: How do we ensure that your body makes the exact ones that we need to protect against flu and HIV? The principal challenge for both of these viruses is that they're always changing. So let's take a look at the flu virus. In this rendering of the flu virus, these different colored spikes are what it uses to infect you. And also, what the antibodies use is a handle to essentially grab and neutralize the virus. When these mutate, they change their shape, and the antibodies don't know what they're looking at anymore. So that's why every year you can catch a slightly different strain of flu. It's also why in the spring, we have to make a best guess at which three strains are going to prevail the next year, put those into a single vaccine and rush those into production for the fall.
Set Berkli: zaista odličan video, zar ne? Antitela u akciji, koje ste malopre videli na ovom snimku, su upravo ona koja omogućuju rad većini vakcina. Zapravo je pravo pitanje: kako možemo osigurati da vaše telo proizvodi tačno ona antitela koja su nam potrebna za zaštitu protiv gripa i HIV-a? Glavni izazov za oba ova virusa je taj da se oni uvek menjaju. Pogledajmo na virus gripa. U ovom prikazu virusa gripa, ovi, različito obojeni, šiljci su ti koje koristi da bi vas zarazio. Takođe i, ono što antitela koriste je ručica prvenstveno da uhvate i neutrališu virus. Kada oni mutiraju, promene svoj oblik, tako da antitela više ne znaju na šta gledaju. Upravo zbog toga svake godine možede dobiti malčice drugačiji oblik gripa. Takođe zbog toga na proleće, moramo nagađati koji oblici će biti dominantan sledeće godine, staviti ih u vakcine i dati ih u proizvodnju za jesen.
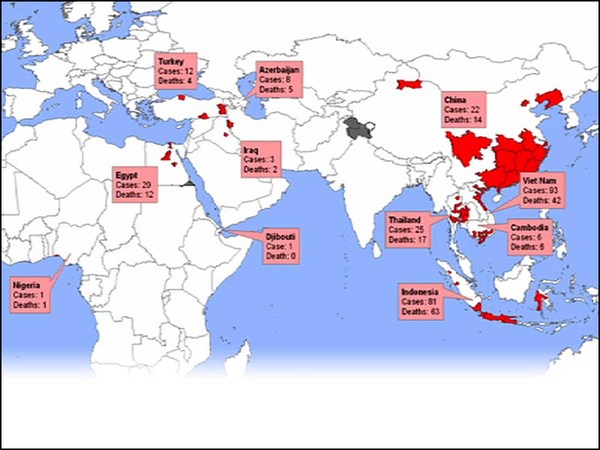
Even worse, the most common influenza -- influenza A -- also infects animals that live in close proximity to humans, and they can recombine in those particular animals. In addition, wild aquatic birds carry all known strains of influenza. So, you've got this situation: In 2003, we had an H5N1 virus that jumped from birds into humans in a few isolated cases with an apparent mortality rate of 70 percent. Now luckily, that particular virus, although very scary at the time, did not transmit from person to person very easily. This year's H1N1 threat was actually a human, avian, swine mixture that arose in Mexico. It was easily transmitted, but, luckily, was pretty mild. And so, in a sense, our luck is holding out, but you know, another wild bird could fly over at anytime.
Još gore, najčešći grip -- grip A -- takođe inficira i životinje koje žive u ljudskoj blizini, i koji se mogu rekombinovati u tim određenim životinjama. Dodatno, divlje vodene ptice nose sve poznate oblike gripa. Tako da imate sledeću situaciju: imali smo 2003. godine H5N1 virus koji je prešao sa ptica na ljude u nekoliko izolovanih slučajeva sa jasnom stopom smrtnosti od sedamdeset odsto. Srećom, ovaj poseban virus, iako jako strašan u to vreme, nije se prenosio sa osobe na osobu tako lako. Ovogodišnja pretnja H1N1 je zapravo bila mešavina ljudskog, ptičjeg i svinjskog gripa koji je nastao u Meksiku. Lako se prenosio, ali, srećom, bio je prilično blag. Tako, u nekom smislu, održava nas sreća, samo da znate, neka druga divlja ptica može preleteti bilo kada.
Now let's take a look at HIV. As variable as flu is, HIV makes flu look like the Rock of Gibraltar. The virus that causes AIDS is the trickiest pathogen scientists have ever confronted. It mutates furiously, it has decoys to evade the immune system, it attacks the very cells that are trying to fight it and it quickly hides itself in your genome. Here's a slide looking at the genetic variation of flu and comparing that to HIV, a much wilder target. In the video a moment ago, you saw fleets of new viruses launching from infected cells. Now realize that in a recently infected person, there are millions of these ships; each one is just slightly different. Finding a weapon that recognizes and sinks all of them makes the job that much harder.
Pogledajmo sada HIV. Iako promenljiv kao grip, HIV čini da grip izgleda kao malo ispupčenje. Virus koji uzrokuje SIDU je najprevarljiviji patogen kome su se naučnici ikada suprotstavili. On opasno mutira, ima mamce za izbegavanje imunog sistema, napada same ćelije koje pokušavaju da se bore sa njim i brzo se sakriva u vašem genomu. Evo slajda sa pogledom na genetsku varijaciju gripa i upoređujući to sa HIV-om, mnogo divljijom metom. U snimku pre nekoliko momenata, videli ste flote novih virusa lansiranih iz zaraženih ćelija. Shvatite sada da u nedavno zaraženoj osobi, postoje milioni ovih brodova; svaki je samo malčice drugačiji. Pronaći oružie koji ih prepoznaje i koje ih sve potapa čini posao mnogo težim.
Now, in the 27 years since HIV was identified as the cause of AIDS, we've developed more drugs to treat HIV than all other viruses put together. These drugs aren't cures, but they represent a huge triumph of science because they take away the automatic death sentence from a diagnosis of HIV, at least for those who can access them. The vaccine effort though is really quite different. Large companies moved away from it because they thought the science was so difficult and vaccines were seen as poor business. Many thought that it was just impossible to make an AIDS vaccine, but today, evidence tells us otherwise.
Sada, 27 godina nakon identifikacije HIV-a kao uzročnika SIDE, mi smo razvili više lekova za tretman HIV-a nego za sve druge viruse zajedno. Ovi lekovi ne leče, već predstavljaju veliki trijumf nauke jer oduzimaju automatsku smrtnu kaznu od dijagnoze HIV-a, bar za one koji mogu doći do njih. Dejstvo vakcine je zapravo dosta drugačije. Velike kompanije su se udaljile od njih jer su mislile da je nauka jako teška i vakcine su izgledale kao slab biznis. Mnogi su mislili da je nemoguće proizvesti vakcinu protiv SIDE, međutim, danas nam dokazi drugačije govore.
In September, we had surprising but exciting findings from a clinical trial that took place in Thailand. For the first time, we saw an AIDS vaccine work in humans -- albeit, quite modestly -- and that particular vaccine was made almost a decade ago. Newer concepts and early testing now show even greater promise in the best of our animal models. But in the past few months, researchers have also isolated several new broadly neutralizing antibodies from the blood of an HIV infected individual. Now, what does this mean? We saw earlier that HIV is highly variable, that a broad neutralizing antibody latches on and disables multiple variations of the virus. If you take these and you put them in the best of our monkey models, they provide full protection from infection. In addition, these researchers found a new site on HIV where the antibodies can grab onto, and what's so special about this spot is that it changes very little as the virus mutates. It's like, as many times as the virus changes its clothes, it's still wearing the same socks, and now our job is to make sure we get the body to really hate those socks.
U septembru, imali smo iznanađujuće i uzbuđujuće zaključke iz kliničkog ispitivanja koje je bilo na Tajlandu. Po prvi put, videli smo rad vakcina protiv SIDE na ljudima -- mada, prilično skromno -- i baš ta vakcina je napravljena skoro pre deset godina. Noviji koncepti i rana testiranja pokazuju sada mnogo veća obećanja u našim najboljim životinjskim modelima. U proteklih nekoliko meseci, istraživači su takođe izolovali nekoliko novih, neutralizovanih antitela iz krvi HIV-pozitivnog pojedinca. Sada, što to znači? Videli smo da je HIV jako promenjljiv, da se široko neutralizujuće antitelo zakači i onemogući višestruke promene virusa. Ako ih stavite na najbolje modele majmuna, oni pružaju potpunu zaštitu od zaraze. Pored toga, ovi istraživači su našli novo mesto na HIV-u za koje se mogu uhvatiti antitela, i ono što je specifično za ovo mesto je da se jako malo menja pri mutaciji virusa. To je kao, koliko se puta virus presvuče, on uvek nosi iste čarape, pa je sada naš posao da osiguramo da telo zaista zamrzi te čarape.
So what we've got is a situation. The Thai results tell us we can make an AIDS vaccine, and the antibody findings tell us how we might do that. This strategy, working backwards from an antibody to create a vaccine candidate, has never been done before in vaccine research. It's called retro-vaccinology, and its implications extend way beyond that of just HIV. So think of it this way. We've got these new antibodies we've identified, and we know that they latch onto many, many variations of the virus. We know that they have to latch onto a specific part, so if we can figure out the precise structure of that part, present that through a vaccine, what we hope is we can prompt your immune system to make these matching antibodies. And that would create a universal HIV vaccine. Now, it sounds easier than it is because the structure actually looks more like this blue antibody diagram attached to its yellow binding site, and as you can imagine, these three-dimensional structures are much harder to work on. And if you guys have ideas to help us solve this, we'd love to hear about it.
Tako da je to problem. Rezultati sa Tajlanda nam ukazuju da možemo praviti vakcine protiv SIDE, dok nam pronalasci o antitelima govore o tome kako to možemo učiniti. Ovakva strategija, radeći unatraške od antitela praviti vakcina, nikada ranije nije bila urađena u istraživanju vakcina. Zove se retro-vakcinacija, i njene primene se protežu mnogo dalje od HIV-a. Razmišljajte ovako. Imamo ova nova antitela koje smo identifikovali, i znamo da se ona pričvršćuju na mnoge, mnoge varijacije virusa. Znamo da se moraju pričvrstiti na određen deo, ako bi mogli da otkrijemo tačnu strukturu tog dela, predstavljenog putem vakcina, ono čemu se nadamo je da možemo brzo navesti vaš imun sistem da pravi ova odgovarajuća antitela. To bi stvorilo univerzalnu vakcinu protiv HIV-a. Ovo zvuči lakše nego što jeste zato što struktura zapravo izgleda više kao ovaj plavi dijagram antitela zakačen na svoje vezivno žuto mesto, i kao što možete pretpostaviti, rad na ovim trodimenzionim strukturama je mnogo teži. Ako neko od vas ima ideje kako bi nam pomogao da rešimo ovo, rado bismo vas saslušali.
But, you know, the research that has occurred from HIV now has really helped with innovation with other diseases. So for instance, a biotechnology company has now found broadly neutralizing antibodies to influenza, as well as a new antibody target on the flu virus. They're currently making a cocktail -- an antibody cocktail -- that can be used to treat severe, overwhelming cases of flu. In the longer term, what they can do is use these tools of retro-vaccinology to make a preventive flu vaccine. Now, retro-vaccinology is just one technique within the ambit of so-called rational vaccine design.
Međutim, znate, istraživanje koje se vršilo za HIV sada je zaista pomoglo i sa inovacijom za druge bolesti. Tako na primer, kompanije biotehnologije su sada pronašla široko neutralizujuća antitela od gripa, kao i nove mete antitela na virus gripa. Oni trenutno prave koktel -- koktel antitela -- koji bi mogao da se koristi za lečenje ozbiljnih, nadmoćnih slučajeva gripa. Na duži period, oni mogu da iskoriste alate retro-vakcinacije za pravljenje preventivnih vakcina od gripa. Sada, reto-vakcinacija je samo jedna tehnika u polju, takozvanih racionalnih dizajna vakcina.
Let me give you another example. We talked about before the H and N spikes on the surface of the flu virus. Notice these other, smaller protuberances. These are largely hidden from the immune system. Now it turns out that these spots also don't change much when the virus mutates. If you can cripple these with specific antibodies, you could cripple all versions of the flu. So far, animal tests indicate that such a vaccine could prevent severe disease, although you might get a mild case. So if this works in humans, what we're talking about is a universal flu vaccine, one that doesn't need to change every year and would remove the threat of death. We really could think of flu, then, as just a bad cold.
Dozvolite mi da vam dam još jedan primer. Ranije smo pričali od H i N šiljcima na površini virusa gripa. Primetite ove druge, manje izbočine. One su uglavnom sakrivene od imunog sistema. Ispostavlja se sada da se ove tačke takođe ne menjaju mnogo pri mutaciji virusa. Ako bi se one mogle onesposobiti određenim antitelima, mogle bi se onesposobiti sve verzije gripa. Za sada, testiranje na životinjama ukazuje da takve vakcine mogu sprečiti teške bolesti, mada se mogu dobiti blaži slučajevi. Ako ovo funkcioniše za ljude, ono o čemu pričamo je univerzalna vakcina protiv gripa, jedna koju ne treba menjati svake godine i koja bi uklonila sve pretnje smrću. Tada bi zaista mogli misliti o gripu, kao o jednoj lošoj prehladi.
Of course, the best vaccine imaginable is only valuable to the extent we get it to everyone who needs it. So to do that, we have to combine smart vaccine design with smart production methods and, of course, smart delivery methods. So I want you to think back a few months ago. In June, the World Health Organization declared the first global flu pandemic in 41 years. The U.S. government promised 150 million doses of vaccine by October 15th for the flu peak. Vaccines were promised to developing countries. Hundreds of millions of dollars were spent and flowed to accelerating vaccine manufacturing. So what happened?
Naravno, najbolje zamišljena vakcina je jedino vredna do te mere da je damo svima kojima je to potrebno. Da bismo to uradili, moramo kombinovati pametan dizajn vakcine i pametne načine proizvodnje i, naravno, pametne načine dostavljanja. Želim da razmislite unazad par meseci, U junu, Svetska zdravstvena organizacija je objavila prvu globalnu pandemiju gripa u protekle četrdeset jednu godinu. Vlada SAD-a je obećala sto pedeset miliona doza vakcina do petnaestog oktobra, kada je vrhunac gripa. Vakcine su obećane zemljama u razvoju. Potrošeno je stotine miliona dolara i teklo je ubrzavanje proizvodnje vakcina. Šta se desilo?
Well, we first figured out how to make flu vaccines, how to produce them, in the early 1940s. It was a slow, cumbersome process that depended on chicken eggs, millions of living chicken eggs. Viruses only grow in living things, and so it turned out that, for flu, chicken eggs worked really well. For most strains, you could get one to two doses of vaccine per egg. Luckily for us, we live in an era of breathtaking biomedical advances. So today, we get our flu vaccines from ... chicken eggs, (Laughter) hundreds of millions of chicken eggs. Almost nothing has changed. The system is reliable but the problem is you never know how well a strain is going to grow. This year's swine flu strain grew very poorly in early production: basically .6 doses per egg. So, here's an alarming thought. What if that wild bird flies by again? You could see an avian strain that would infect the poultry flocks, and then we would have no eggs for our vaccines. So, Dan [Barber], if you want billions of chicken pellets for your fish farm, I know where to get them. So right now, the world can produce about 350 million doses of flu vaccine for the three strains, and we can up that to about 1.2 billion doses if we want to target a single variant like swine flu. But this assumes that our factories are humming because, in 2004, the U.S. supply was cut in half by contamination at one single plant. And the process still takes more than half a year.
Prvo smo shvatili kako napraviti vakcine protiv gripa, kako ih proizvoditi, ranih 1940-ih godina. Bio je to spori, ogroman proces koji je zavisio od kokošijih jaja, od miliona živih kokošijih jaja. Virusi rastu samo u živim stvarima, tako da se ispostavilo da su kokošija jaja za grip, obavljala dobar posao. Za većinu vrsta, mogli ste dobiti jednu do dve doze vakcine po jajetu. Srećom po nas, živimo u eri neverovatnih biomedicinskih napredaka. Tako da danas, dobijamo vakcine gipa od ... kokošijih jaja, (smeh) stotina miliona kokošijih jaja. Skoro se ništa nije promenilo. Sistem je pouzdan problem je u tome što nikada ne znate kako će dobro vrsta da izraste. Ove godine vrsta svinjskog gripa je rasla jako slabo u ranoj proizvodnji: u osnovi, 6 doza po jajetu. Evo uznemirujuće pomisli. Šta ako ta divlja ptica opry poleti? Mogli biste videti novu vrstu ptičjeg gripa koji bi zarazio živinu, i tada ne bismo imali jaja za naše vakcine. Dakle, Den [berberin], ako želite milijarde kokošjih peleta za vaš ribnjak, znam gde ih možete nabaviti. Upravo sada, svet može proizvoditi oko 350 miliona doza vakcina od gripa za ove tri vrste, a može se doći do 1.2 milijardi doza ako želimo da napadnemo jednu varijantu kao što je sivinjski grip- Ali ovo pretpostavlja da naše fabrike bruje jer u 2004 godini, snabdevanje iz SAD-a je bilo prepolovljeno kontaminacijom jedne biljke. Procesu još uvek treba više od pola godine.
So are we better prepared than we were in 1918? Well, with the new technologies emerging now, I hope we can say definitively, "Yes." Imagine we could produce enough flu vaccine for everyone in the entire world for less than half of what we're currently spending now in the United States. With a range of new technologies, we could. Here's an example: A company I'm engaged with has found a specific piece of the H spike of flu that sparks the immune system. If you lop this off and attach it to the tail of a different bacterium, which creates a vigorous immune response, they've created a very powerful flu fighter. This vaccine is so small it can be grown in a common bacteria, E. coli. Now, as you know, bacteria reproduce quickly -- it's like making yogurt -- and so we could produce enough swine origin flu for the entire world in a few factories, in a few weeks, with no eggs, for a fraction of the cost of current methods.
Jesmo li spremniji nego što smo bili pre 1918.? Zbog novih tehnologija koje su sada u razvoju, nadam se da možemo konačno reći, ''Da.'' Zamislite da možemo proizvesti dovoljno vakcina sa svakoga na celom svetu za upola manje od onoga što sada trošimo u SAD-u. Uz niz novih tehnologija, mogli bismo. Evo primera: kompanije u kojoj radim je pronašla specifičan deo H šiljka gripa koji podstiče imuni sistem. Ako ovo promenite i zakačite za kraj različitu bakteriju, koja stvara energičan imuni odgovor, napravili ste veoma moćnog borca protiv gripe. Ova vakcina je toliko mala može se uzgajiti na običnoj bakteriji Ešerihija koli. Kao što znate, bakterije se reprodukuju brže -- to je kao pravljenje jogurta -- tako da možemo napraviti dovoljno gripa svinjskog porekla za ceo svet u novim fabrikama, za nekoliko nedelja, bez jaja, za samo deo troškova od današnjih metoda.
(Applause)
(aplauz)
So here's a comparison of several of these new vaccine technologies. And, aside from the radically increased production and huge cost savings -- for example, the E. coli method I just talked about -- look at the time saved: this would be lives saved. The developing world, mostly left out of the current response, sees the potential of these alternate technologies and they're leapfrogging the West. India, Mexico and others are already making experimental flu vaccines, and they may be the first place we see these vaccines in use. Because these technologies are so efficient and relatively cheap, billions of people can have access to lifesaving vaccines if we can figure out how to deliver them.
Evo poređenja nekoliko ovih novih tehnologija vakcina. Pored radikalno ubrzane proizvodnje i velike uštede -- na primer, metodom Ešerihija koli o kojoj sam malo pre pričao -- pogledajte ušteđeno vreme: ovo bi bili spašeni životi. Svet u razvitku, uglavnom izostavljen iz trenutne reakcije, vidi potencijal ovih alternativnih tehnologija i njihovog skoka na zapad. Indija, Meksiko i drugi, već prave eksperimentalne vakcine od gripa, i mogu biti prvo mesto gde ćemo videti korišćenje vakcina. Zbog toga što su ove tehnologije jako efikasne i relativno jeftine, milijarde ljudi mogu imati vakcine koje spašavaju život ako smislimo kako da ih razdelimo.
Now think of where this leads us. New infectious diseases appear or reappear every few years. Some day, perhaps soon, we'll have a virus that is going to threaten all of us. Will we be quick enough to react before millions die? Luckily, this year's flu was relatively mild. I say, "luckily" in part because virtually no one in the developing world was vaccinated. So if we have the political and financial foresight to sustain our investments, we will master these and new tools of vaccinology, and with these tools we can produce enough vaccine for everyone at low cost and ensure healthy productive lives. No longer must flu have to kill half a million people a year. No longer does AIDS need to kill two million a year. No longer do the poor and vulnerable need to be threatened by infectious diseases, or indeed, anybody. Instead of having Vaclav Smil's "massively fatal discontinuity" of life, we can ensure the continuity of life. What the world needs now are these new vaccines, and we can make it happen.
Razmislimo o tome gde nas ovo vodi. Javljaju se nove zarazne bolesti ili obnavljaju stare svakih nekoliko godina. Jednog dana, možda uskoro, imaćemo virus koji će nam svima zapretiti. Da li ćemo biti dovoljno brzi da reagujemo pre nego što milioni umru? Srećom, ovogodišnji grip je bio relativno blag. Kažem ''srećom'' jer praktično niko u državama u razvitku nije bio vakcinisan. Tako da ako imamo političko i finansijsko predviđanje da održimo naše investicije, ovladaćemo ovim i novim alatkama vakcinacije i sa tim alatima ćemo moći proizvoditi dovoljno vakcina za sve po maloj ceni i osigurati zdrave, produktivne živote. Grip više ne mora ubiti pola miliona ljudi godišnje. SIDA više ne mora ubiti dva miliona ljudi godišnje. Siromašni i osetljivi više ne moraju biti ugroženi zaraznim bolestima, ili niko, zapravo. Umesto da imamo Vaclav Smilove ''masovne pomore'' života, možemo osigurati kontinuitet života. Ono što je sada svetu potrebno su ove vakcine, i mi ih možemo ostvariti.
Thank you very much.
Hvala vam mnogo.
(Applause)
(aplauz)
Chris Anderson: Thank you. (Applause) Thank you. So, the science is changing. In your mind, Seth -- I mean, you must dream about this -- what is the kind of time scale on, let's start with HIV, for a game-changing vaccine that's actually out there and usable?
Kris Anderson: Hvala vam. (aplauz) Hvala vam. Dakle, nauka se menja. Po vašem mišljenju, Set -- mislim, mora da sanjate o tome -- kolika je vremenska skala počnimo od HIV-a, za preokret vakcina, da su zapravo na tržištu i upotrebljive?
SB: The game change can come at any time, because the problem we have now is we've shown we can get a vaccine to work in humans; we just need a better one. And with these types of antibodies, we know humans can make them. So, if we can figure out how to do that, then we have the vaccine, and what's interesting is there already is some evidence that we're beginning to crack that problem. So, the challenge is full speed ahead.
SB: Preokret može doći bilo kad, jer smo pokazali da da sa problem koji sada imamo možemo naterati vakcine da funkcionišu za ljude: samo su nam potrebne bolje. Znamo da ljudi mogu proizvesti ove vrste antitela, Tako da, ako shvatimo kako da to uradimo, onda imamo vakcinu, a zanimljivo je da već postoje neki dokazi da smo na početku rešavanja problema. Tako da izazov ide punom brzinom napred.
CA: In your gut, do you think it's probably going to be at least another five years?
KA: Po vašem mišljenju, trebaće verovatno najmanje još pet godina?
SB: You know, everybody says it's 10 years, but it's been 10 years every 10 years. So I hate to put a timeline on scientific innovation, but the investments that have occurred are now paying dividends.
SB: Znate, svi kažu da treba deset godina, ali bilo je, na svakih deset godina, deset godina. Tako da mrzim stavljati periode na naučna otkrića, ali investicije koje su nastale sada plaćaju dividende.
CA: And that's the same with universal flu vaccine, the same kind of thing?
KA: I isto je sa univerzalnom vakcinom od gripa, ista stvar?
SB: I think flu is different. I think what happened with flu is we've got a bunch -- I just showed some of this -- a bunch of really cool and useful technologies that are ready to go now. They look good. The problem has been that, what we did is we invested in traditional technologies because that's what we were comfortable with. You also can use adjuvants, which are chemicals you mix. That's what Europe is doing, so we could have diluted out our supply of flu and made more available, but, going back to what Michael Specter said, the anti-vaccine crowd didn't really want that to happen.
SB: Mislim da je sa gripom drugačije. Mislim da je to šta se događa sa gripom imamo gomilu -- prikazao sam samo nekoliko od njih -- gomilu zaista dobrih i korisnih tehnologija koji su spremni za pokretanje. Izgledaju dobro. Problem je bio što smo mi ulagali u tradicionalne tehnologije jer nam je to odgovaralo. Možete takođe koristiti adjuvante - hemikalije koje izmešate. To je ono što Evropa radi, tako da smo razredili naše zalihe gripa i omogućili ih više dostupnim, dok, vraćajući se na ono što je Majkl Spekter rekao, grupa koja je protiv vakcina zapravo nije želela da se to desi.
CA: And malaria's even further behind?
KA: A malarija je još dalje?
SB: No, malaria, there is a candidate that actually showed efficacy in an earlier trial and is currently in phase three trials now. It probably isn't the perfect vaccine, but it's moving along.
SB: Ne, za malariju postoji kandidat koji se pokazao efikasnim u ranom testiranju i sada je u fazi tri ispitivanja. Najverovatnije nije savršena vakcina, ali napreduje.
CA: Seth, most of us do work where every month, we produce something; we get that kind of gratification. You've been slaving away at this for more than a decade, and I salute you and your colleagues for what you do. The world needs people like you. Thank you.
KA: Set, većina nas radi posao gde svakog meseca, napravi nešto; dobijamo zadovoljstvo. Vi se sa time borite više od decenije, i pozdravljam Vas i vaše kolege zbog onoga što radite. Svetu su potrebni ljudi kao što ste vi. Hvala vam.
SB: Thank you.
SB: Hvala vam.
(Applause)
(aplauz)