At any given moment, trillions of cells are traveling through your blood vessels, sometimes circling the body in just one minute. Each of these cells has its origins deep in your bones. Bones might seem rock-solid, but they’re actually quite porous inside. Large and small blood vessels enter through these holes. And inside most of the large bones of your skeleton is a hollow core filled with soft bone marrow. Marrow contains fat and other supportive tissue, but its most essential elements are blood stem cells. These stem cells are constantly dividing. They can differentiate into red blood cells, white blood cells, and platelets, and send about hundreds of billions of new blood cells into circulation every day. These new cells enter the bloodstream through holes in small capillaries in the marrow. Through the capillaries, they reach larger blood vessels and exit the bone.
Svakog trenutka, bilioni ćelija putuju kroz vaše krvne sudove, ponekad prolazeći celo telo za samo jedan minut. Svaka od ovih ćelija potiče duboko u vašim kostima. Možda se čini da su kosti tvrde kao kamen, ali su zapravo veoma šuplje iznutra. Veliki i mali krvni sudovi ulaze kroz te rupe. Unutar većine velikih kostiju vašeg skeleta je šuplje jezgro ispunjeno mekom koštanom srži. Srž sadrži masti i drugo potporno tkivo, ali njen najbitniji deo jesu matične krvne ćelije. Ove matične ćelije se stalno dele. Mogu se podeliti na crvena krvna zrnca, bela krvna zrnca i trombocite i one šalju stotine milijardi novih krvnih ćelija u krvotok svakog dana. Ove nove ćelije ulaze u krvotok kroz rupe u malim kapilarima u koštanoj srži. Kroz kapilare, one dolaze do većih krvnih sudova i izlaze iz kostiju.
If there’s a problem with your blood, there’s a good chance it can be traced back to the bone marrow. Blood cancers often begin with genetic mutations in the stem cells. The stem cells themselves are not cancerous, but these mutations can interfere with the process of differentiation and result in malignant blood cells. So for patients with advanced blood cancers like leukemia and lymphoma, the best chance for a cure is often an allogeneic bone marrow transplant, which replaces the patient’s bone marrow with a donor’s.
Ako postoji problem sa vašom krvlju, postoji dobra šansa da koren problema leži u koštanoj srži. Rak krvi uglavnom počinje genetskom mutacijom matičnih ćelija. Matične ćelije same po sebi nisu kancerogene, ali ove mutacije mogu da se umešaju u proces diferencijacije i posledica toga su maligne krvne ćelije. Stoga je za pacijente sa rakom krvi u zamakloj fazi poput leukemije i limfoma, najbolje rešenje često transplantacija alogene koštane srži, gde donor daje obolelom pacijentu svoju koštanu srž.
Here’s how it works. First, blood stem cells are extracted from the donor. Most commonly, blood stem cells are filtered out of the donor’s bloodstream by circulating the blood through a machine that separates it into different components. In other cases, the marrow is extracted directly from a bone in the hip, the iliac crest, with a needle.
To funkcioniše ovako. Prvo se matične krvne ćelije uzmu od donora. Najčešće se matične krvne ćelije izvuku iz donorovog krvotoka tako što krv cirkuliše u mašini koja razdvaja krv na različite delove. U drugim slučajevima, koštana srž se uzima iglom, direktno iz koske u kuku - ilijačnog grebena. Primalac se u međuvremenu priprema za transplantaciju.
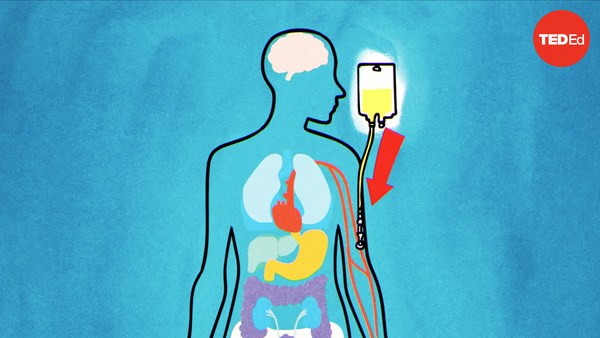
Meanwhile, the recipient prepares for the transplant. High doses of chemotherapy or radiation kill the patient’s existing marrow, destroying both malignant cells and blood stem cells. This also weakens the immune system, making it less likely to attack the transplanted cells. Then the donor cells are infused into the patient’s body through a central line. They initially circulate in the recipient’s peripheral bloodstream, but molecules on the stem cells, called chemokines, act as homing devices and quickly traffic them back to the marrow. Over the course of a few weeks, they begin to multiply and start producing new, healthy blood cells. Just a small population of blood stem cells can regenerate a whole body’s worth of healthy marrow.
Jaka hemoterapija ili velike doze radijacije ubiju postojeću srž pacijenta, ubijajući i maligne ćelije i matične krvne ćelije. Ovo takođe slabi imuni sistem, što smanjuje verovatnoću da će napasti transplantovane ćelije. Zatim se donorove ćelije ubace u telo pacijenta kroz centralnu venu. One u početku cirkulišu u perifernom krvotoku primaoca, ali hemokini, molekuli na matičnim ćelijama, deluju kao uređaji za navođenje i brzo vode krvne ćelije nazad u srž. Tokom perioda od nekoliko nedelja one počinju da se razmnožavaju i da proizvode nove, zdrave krvne ćelije. Samo mali broj matičnih krvnih ćelija može da proizvede zdravu srž za celo telo.
A bone marrow transplant can also lead to something called graft-versus-tumor activity, when new immune cells generated by the donated marrow can wipe out cancer cells the recipient’s original immune system couldn’t. This phenomenon can help eradicate stubborn blood cancers. But bone marrow transplants also come with risks, including graft-versus-host disease. It happens when the immune system generated by the donor cells attacks the patient’s organs. This life-threatening condition occurs in about 30–50% of patients who receive donor cells from anyone other than an identical twin, particularly when the stem cells are collected from the blood as opposed to the bone marrow.
Transplantacija koštane srži takođe može dovesti do nečega što se naziva kalem protiv tumora efektom, gde nove imune ćelije koje je proizvela donorova srž mogu ubiti ćelije raka koje prvobitni imuni sistem primaoca nije mogao. Ovaj fenomen može doprineti iskorenjivanju upornog raka krvi. Međutim, transplantacije koštane srži imaju i svoje rizike, uključujući i bolest kalem protiv domaćina. Do toga dolazi kada imuni sistem koji su sagradile ćelije donora napadne pacijentove organe. Ova smrtonosna bolest događa se kod oko 30 do 50 procenata pacijenata koji prime ćelije od bilo koga ko nije njihov jednojajčani blizanac, posebno ako su matične ćelije uzete iz krvi, a ne iz koštane srži.
Patients may take immunosuppressant medications or certain immune cells may be removed from the donated sample in order to reduce the risk of graft-versus-host disease. But even if a patient avoids graft-versus-host disease, their immune system may reject the donor cells. So it’s crucial to find the best match possible in the first place.
Pacijenti mogu uzeti imunosupresivne lekove, ili se određene imunoćelije mogu ukloniti iz doniranog uzorka kako bi se smanjio rizik od bolesti kalem protiv domaćina. Međutim, čak iako pacijent izbegne bolest kalem protiv domaćina, njegov imuni sistem može odbiti donorove ćelije. Stoga je pre svega ključno pronaći najboljeg mogućeg donora.
Key regions of the genetic code determine how the immune system identifies foreign cells. If these regions are similar in the donor and the recipient, the recipient’s immune system is more likely to accept the donor cells. Because these genes are inherited, the best matches are often siblings. But many patients who need a bone marrow transplant don’t have a matched family member. Those patients turn to donor registries of volunteers willing to offer their bone marrow.
Važni delovi genetskog koda određuju kako imuni sistem identifikuje strane ćelije. Ako su ti delovi slični kod donora i kod primaoca, veća je verovatnoća da će imuni sistem primaoca prihvatiti ćelije donora. Zato što se ovi geni nasleđuju, najveće podudaranje će biti između braće i sestara. Međutim, mnogi pacijenti kojima je potrebna transplantacija srži nemaju člana porodice koji bi mogao biti donor. Ti pacijenti se obraćaju registrima donora gde se mogu naći ljudi koji bi dobrovoljno dali koštanu srž.
All it takes to be on the registry is a cheek swab to test for a genetic match. And in many cases, the donation itself isn’t much more complicated than giving blood. It’s a way to save someone’s life with a resource that’s completely renewable.
Sve što je potrebno da se nađete u registru jeste bris usta kojim se testira genetska podudarnost. U mnogim slučajevima samo doniranje nije ništa komplikovanije od davanja krvi. To je način da spasite nečiji život