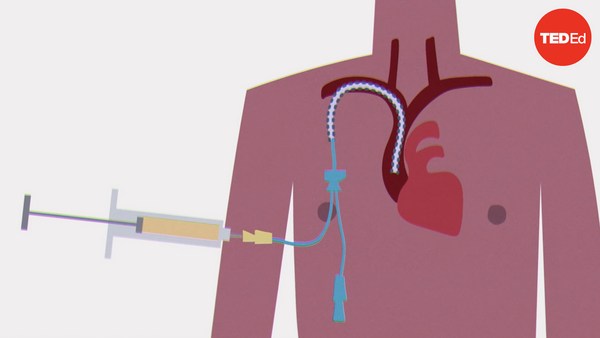
In 1881, doctor William Halsted rushed to help his sister Minnie, who was hemorrhaging after childbirth. He quickly inserted a needle into his arm, withdrew his own blood, and transferred it to her. After a few uncertain minutes, she began to recover.
Godine 1881, doktor Vilijam Halsted žurio je da pomogne svojoj sestri Mini, koja je krvarila nakon porođaja. Brzo je ubacio iglu u svoju ruku, izvadio je svoju krv i dao je sestri. Nakon nekoliko neizvesnih minuta, počela je da se oporavlja.
Halsted didn’t know how lucky they’d gotten. His transfusion only worked because he and his sister happened to have the same blood type— something that isn’t guaranteed, even among close relatives.
Halsted nije znao koliko su imali sreće. Njegova transfuzija je uspela samo zato što su on i njegova sestra imali istu krvnu grupu, nešto što nije zagarantovano, čak i među užom rodbinom.
Blood types hadn’t been discovered by Halsted’s time, though people had been experimenting with transfusions for centuries— mostly unsuccessfully. In 1667, a French physician named Jean-Baptiste Denis became the first to try the technique on a human. Denis transfused sheep’s blood into Antoine Mauroy, a man likely suffering from psychosis, in the hopes that it would reduce his symptoms. Afterward, Mauroy was in good spirits. But after a second transfusion, he developed a fever, severe pain in his lower back, intense burning in his arm, and he urinated a thick, black liquid.
Krvne grupe nisu bile otkrivene u Halstedovo vreme, iako su ljudi eksperimentisali sa transfuzijama vekovima, uglavnom bezuspešno. Godine 1667, francuski lekar Žan-Baptist Deni je postao prvi koji je pokušao tehniku na ljudskom biću. Deni je preneo krv ovce u Antoena Moroa, čoveka koji je verovatno patio od psihoze, u nadi da će smanjiti njegove simptome. Nakon toga, Moro je bio raspoložen. Ali nakon druge transfuzije, dobio je temperaturu, jak bol u donjem delu leđa, intenzivno pečenje u ruci i mokrio je gustu, crnu tečnost.
Though nobody knew it at the time, these were the signs of a dangerous immune response unfolding inside his body. This immune response starts with the production of proteins called antibodies, which distinguish the body’s own cells from intruders. They do so by recognizing the foreign proteins, or antigens, embedded in an intruder’s cell membrane. Antibodies latch onto the antigens, signaling other immune cells to attack and destroy the foreign cells.
Niko nije znao u to vreme, pak, da su ovo bili znaci opasne imune reakcije koja se odvijala unutar njegovog tela. Ovaj imuni odgovor započinje proizvodnjom proteina koji se nazivaju antitelima, koja prave razliku između ćelija sopstvenog tela i uljeza. To rade tako što prepoznaju strane proteine ili antigene, koji su ugrađeni u ćelijsku membranu uljeza. Antitela se zakače za antigene, dajući signal ostalim imunim ćelijama da napadnu i unište strane ćelije.
The destroyed cells are flushed from the body in urine. In extreme cases, the massive break down of cells causes clots in the bloodstream that disrupt the flow of blood to vital organs, overload the kidneys, and cause organ failure. Fortunately, Denis’s patient survived the transfusion. But, after other cross-species transfusions proved fatal, the procedure was outlawed across Europe, falling out of favor for several centuries.
Uništene ćelije se izbacuju iz tela kroz urin. U ekstremnim slučajevima, masovno razlaganje ćelija uzrokuje ugruške u krvnom toku, koji remete tok krvi ka vitalnim organima, preopterećuju bubrege i uzrokuju otkazivanje organa. Na sreću, Denijev pacijent je preživeo transfuziju. Ali, nakon što su se druge transfuzije između vrsta pokazale fatalnim, procedura je postala zabranjena duž Evrope i nije se koristila nekoliko vekova.
It wasn’t until 1901 that Austrian physician Karl Landsteiner discovered blood types, the crucial step in the success of human to human blood transfusions. He noticed that when different types were mixed together, they formed clots. This happens when antibodies latch on to cells with foreign antigens, causing blood cells to clump together. But if the donor cells are the same blood type as the recipient’s cells, the donor cells won’t be flagged for destruction, and won’t form clumps.
Sve do 1901. godine kada je austrijski lekar Karl Landštajner otkrio krvne grupe, važan korak ka uspešnoj transfuziji krvi između ljudi. Primetio je da kada se pomešaju različite grupe, one prave ugruške. Ovo se dešava kada se antitela zakače za ćelije sa stranim antigenima, uzrokujući da se ćelije krvi zgrušaju. Ali, ako su ćelije donora iste krvne grupe kao ćelije primaoca, ćelije donora neće biti uništene i neće se formirati grudvice.
By 1907, doctors were mixing together small amounts of blood before transfusing it. If there were no clumps, the types were a match. This enabled them to save thousands of lives, laying the foundation for modern transfusions.
Do 1907. godine, doktori su mešali male količine krvi pre nego što je transfundiraju. Ako nije bilo grudvica, tipovi su se poklapali. Ovo im je omogućilo da spasu hiljade života, postavljajući temeljac za moderne transfuzije.
Up to this point, all transfusions had occurred in real time, directly between two individuals. That’s because blood begins to clot almost immediately after coming into contact with air— a defense mechanism to prevent excessive blood loss after injury.
Sve do sada, sve transfuzije su se dešavale u sadašnjem vremenu, direktno između dve individue. To je zato što krv počinje da se zgrušava skoro odmah nakon što dođe u kontakt sa vazduhom, a to je odbrambeni mehanizam koji sprečava prekomerno gubljenje krvi nakon povrede.
In 1914, researchers discovered that the chemical sodium citrate stopped blood coagulating by removing the calcium necessary for clot formation. Citrated blood could be stored for later use— the first step in making large scale blood transfusions possible. In 1916, a pair of American scientists found an even more effective anticoagulant called heparin, which works by deactivating enzymes that enable clotting. We still use heparin today.
Godine 1914, istraživači su otkrili da hemikalija natrijum citrat zaustavlja koagulaciju krvi otklanjajući kalcijum koji je neophodan za zgrušavanje. Krv sa citratima može da se sačuva za kasniju upotrebu, što je prvi korak ka omogućavanju transfuzije krvi u velikim razmerama. Godine 1916, par američkih naučnika je otkrio efektniji antikoagulant nazvan heparin koji deaktivira enzime koji omogućuju zgrušavanje. I dan-danas koristimo heparin.
At the same time, American and British researchers developed portable machines that could transport donor blood onto the battlefields of World War I. Combined with the newly-discovered heparin, medics safely stored and preserved liters of blood, wheeling it directly onto the battlefield to transfuse wounded soldiers.
U isto vreme, američki i britanski istraživači su razvili prenosive mašine koje su mogle da transportuju krv na bojna polja u Prvom svetskom ratu. U kombinaciji sa novootkrivenim heprinom, doktori su na siguran način skladištili i čuvali litre krvi, prebacujući je direktno na bojno polje da daju krv ranjenim vojnicima.
After the war, this crude portable box would become the inspiration for the modern-day blood bank, a fixture of hospitals around the world.
Nakon rata, ova nezgrapna prenosiva kutija postala je inspiracija za današnju banku krvi, i deo je opreme bolnica širom sveta.