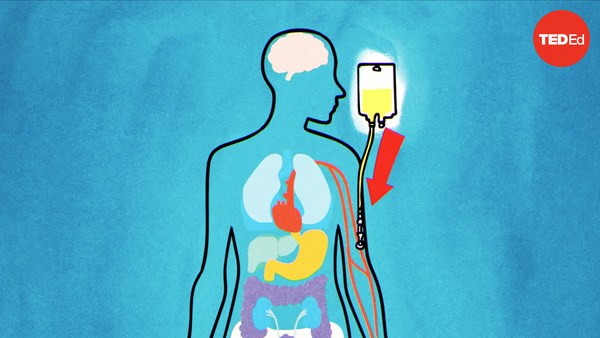
London, 1928: a group of mold spores surf a breeze through a lab. They drift onto a petri dish, and when they land, they germinate a medical revolution. This lab belongs to Alexander Fleming, a Scottish scientist investigating the properties of infectious bacteria. At this time, Fleming is away on vacation. When he returns, he finds a colony of mold growing on a petri dish he’d forgotten to place in his incubator. And around this colony of mold is a zone completely and unexpectedly clear of bacteria.
London, 1928. godine, spore buđi vetrom su dospele do laboratorije. Nanele su se na petrijevu posudu, a kada su se spustile, proklijala je medicinska revolucija. Ova laboratorija je pripadala Aleksandru Flemingu, škotskom naučniku koji je istraživao svojstva zaraznih bakterija. U to vreme, Fleming je bio na putu. Kada se vratio, našao je koloniju buđi koja se razmnožava u petrijevoj posudi, a koju je zaboravio da stavi u inkubator. Oko ove kolonije buđi je bila zona koja je potpuno i neočekivano bila bez bakterija.
In studying this mysterious phenomenon, Fleming came to realize that the mold was secreting some kind of compound that was killing the bacteria. The mold was a species in the Penicillium genus, so Fleming dubbed the antibacterial compound “penicillin.”
Istražujući ovu misterioznu pojavu, Fleming je došao do saznanja da buđ luči neko jedinjenje koje ubija bakterije. Buđ je vrsta u rodu peniciliuma, tako da je Fleming nazvao antibakterijsko jedinjenje penicilin.
What Fleming stumbled upon was a microbial defense system. The penicillium mold constantly produces penicillin in order to defend itself from threats, such as nearby bacterial colonies that might consume its resources. Penicillin destroys many types of bacteria by disrupting synthesis of their cell walls. These walls get their strength from a thick, protective mesh of sugars and amino acids, that are constantly being broken down and rebuilt. Penicillin binds to one of the compounds that weaves this mesh together and prevents the wall from being reconstructed at a critical phase. Meanwhile, penicillin stimulates the release of highly reactive molecules that cause additional damage. Eventually, the cell’s structure breaks down completely. This two-pronged attack is lethal to a wide range of bacteria, whether in petri-dishes, our bodies, or elsewhere. It’s not, however, harmful to our own cells, because those don’t have cell walls.
Fleming je naišao na mikrobski odbrambeni mehanizam. Buđ peniciliuma neprestano proizvodi penicilin da bi se odbranila od pretnji, kao što su obližnje kolonije bakterija koje mogu da potroše njene resurse. Penicilin uništava mnogo tipova bakterija tako što ometa sintezu njihovog zida ćelija. Ovi zidovi dobijaju snagu od debele, zaštitne mreže šećera i aminokiselina, koje se neprestano rastavljaju i ponovo sastavljaju. Penicilin se vezuje za jedno od jedinjenja koja tkaju ovu mrežu zajedno i sprečava da se zid ponovo izgradi u kritičnoj fazi. U međuvremenu, penicilin stimuliše otpuštanje veoma reaktivnih molekula koji uzrokuju dodatna oštećenja. Na kraju, struktura ćelije se potpuno raspada. Ovaj dvokraki napad je smrtonosan za širok opseg bakterija, bilo da su u petrijevoj posudi, našim telima ili bilo gde drugde. Nije, međutim, štetan za naše ćelije, jer one nemaju zidove ćelija.
For a decade or so after Fleming’s discovery, penicillin remained a laboratory curiosity. But during World War II, researchers figured out how to isolate the active compound and grow the mold in larger quantities. They then went on to win the Nobel Prize for their work. Teams at Oxford and several American drug companies continued development, and within a few years it was commercially available. Penicillin and similar compounds quickly transformed the treatment of infections. For the time being, they remain some of the most important, life-saving antibiotics used in medicine.
Oko jedne decenije nakon Flemingovog otkrića, penicilin je ostao laboratorijska znatiželja. Ali tokom Drugog svetskog rata, naučnici su shvatili kako da izoluju aktivno jedinjenje i razmnožavaju buđ u velikim količinama. Oni su osvojili Nobelovu nagradu za svoj rad. Timovi na Oksfordu i nekoliko američkih kompanija za lekove su nastavili razvoj, i u roku od par godina bio je u slobodnoj prodaji. Penicilin i slična jedinjenja su brzo promenili lečenje infekcija. Za sada, oni su i dalje najvažniji antibiotici korišćeni u medicini.
However, the more we use any antibiotic, the more bacteria evolve resistance to it. In the case of penicillin, some bacteria produce compounds that can break down the key structure that interferes with cell wall synthesis. As antibiotic use has increased, more and more bacteria have evolved this defense, making these antibiotics ineffective against a growing number of bacterial infections. This means it’s essential that doctors not overprescribe the drug.
Međutim, što više koristimo antibiotike, to bakterije postaju rezistentnije. U slučaju penicilina, neke bakterije proizvode jedinjenja koja mogu da razbiju ključnu strukturu koja sprečava sintezu zida ćelije. Kako se korišćenje antibiorika povećalo, sve više i više bakterija je postalo rezistentno čineći ove antibiotike nedelotvornim protiv rastućeg broja bakterijskih infekcija. Ovo znači da je važno da doktori ne prepisuju previše lekova.
Meanwhile, 5 to 15% of patients in developed countries self-identify as allergic to penicillin, making it the most commonly reported drug allergy. However, the vast majority— over 90%— of people who think they’re allergic to penicillin actually are not. Why the misperception? Many patients acquire the allergy label as children, when a rash appears after they’re treated for an infection with penicillin or closely related drugs. The rash is often blamed on penicillin, while the more likely culprit is the original infection, or a reaction between the infection and the antibiotic. However, genuine penicillin allergies, where our immune systems mistake penicillin for an attacker, do occur rarely and can be very dangerous. So if you think you’re allergic but don’t know for sure, your best bet is to visit an allergist. They’ll complete an evaluation that’ll confirm whether or not you have the allergy.
Pet do 15 procenata pacijenata u razvijenim zemljama sami sebi daju dijagnozu da imaju alergiju na penicilin, čineći je najčešćom alergijom na lekove. Međutim, većina ljudi, preko 90 procenata, koji misle da su alergični na penicilin zapravno nisu. Čemu pogrešna percepcija? Mnogi pacijenti steknu alergije kao deca, kada se pojavi osip nakon terapije penicilina ili lekova iz iste familije. Često se krivi penicilin za osip, dok je verovatniji krivac prvobitna infekcija ili reakcija između infekcije i antibiotika. Stvarna alergija na penicilin, to je kada naš imuni sistem pomeša penicilin i napadača, se retko dešava i može da bude opasna. Dakle ako mislite da ste alergični ali ne znate zasigurno, najbolje je da posetite alergologa. Oni će izvršiti evaluaciju koja će potvrditi da li imate alergiju ili ne.
Even if you do have a penicillin allergy, your immune cells that react to the drug may lose their ability to recognize it. In fact, about 80% of people who are allergic to penicillin outgrow their allergy within ten years. This is great news for people who currently identify as allergic to penicillin; the drug may one day save their lives, as it has done for so many others.
Čak i ako imate alergiju na penicilin, vaš imune ćelije koje reaguju na lek mogu izgubiti sposobnost da ga prepoznaju. U stvari, oko 80 procenata ljudi koji su alergični na penicilin prerastu svoje alergije u roku od 10 godina. Ovo je velika vest za ljude koji trenutno misle da imaju alergiju na penicilin. Ovaj lek im jednog dana možda spasi živote kao što je to učinio za mnoge druge.