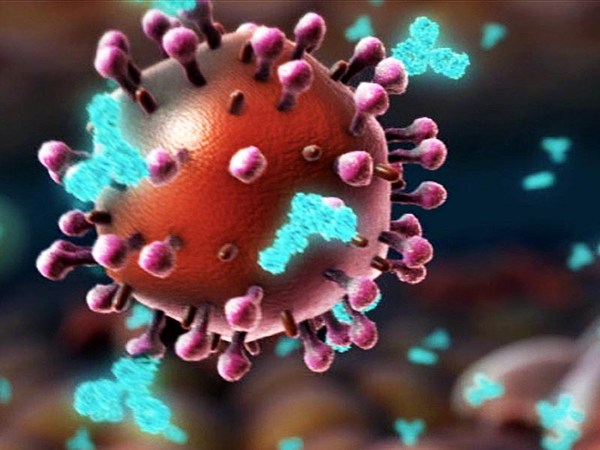
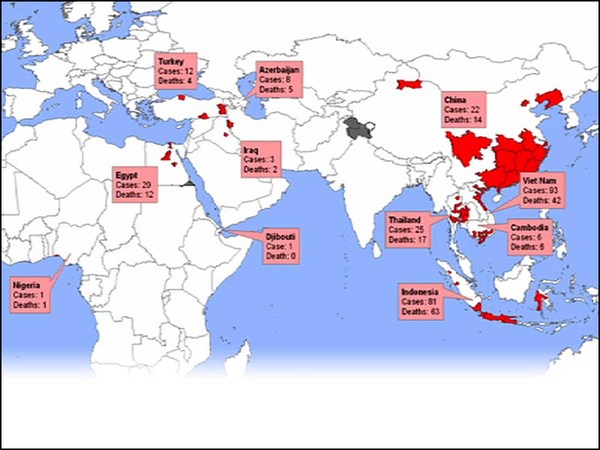
I want to tell you about a student of mine. A few weeks ago, she was on vacation when at 3am she got a phone call. It was her husband telling her that the city that she was in would be quarantined by 10am. She was in Wuhan, China. The epicenter of the coronavirus outbreak. By 8am she was on the road in a friend's car driving 500 miles to Shanghai Airport. The entire time, she was terrified the authorities would arrest her. She made it out on one of the last flights.
我想和大家分享一个我学生的故事。 几周前,她在度假。 凌晨三点的时候她接到一个电话, 电话的那头是她的丈夫, 通知她,她所在的城市 将在上午十点开始被隔离。 她当时在中国武汉, 新冠肺炎病毒爆发的正中心。 早上八点,她已经在朋友的车上, 驶向 500 英里外的上海机场。 她全程处于害怕的状态中。 最终她成功乘上了末班机。
So we're all relieved that she's back home, safe in the US. But what if I told you she was in this room? What if I told you she was sitting next to you? There's no vaccine. There won't be a vaccine for at least 12 months. And this virus is mutating, so there's no guarantee that the vaccine that we produce 12 months from now will match the mutated virus. We're always playing catch-up. And this is the scenario we're in every time there's an outbreak. Our quarantines are porous, our medical responses are flat-footed.
她现在回到美国家中,安然无恙, 我们都松了一口气。 但是假如我告诉你, 她现在就在这里, 她就坐在你旁边呢? 我们当时没有疫苗。 至少 12个 月内都不会有疫苗。 同时病毒在变异, 因此没人能保证 12 月内我们研究出的疫苗 还能应对已经变异的病毒。 我们永远在追赶当中。 每当病毒爆发的时候, 我们都要面临这样的情况。 我们的防疫隔离漏洞百出, 我们的医疗反应措手不及。
The fundamental problem that we face in controlling these outbreaks is that viruses and other infections do two things really well: they mutate and they transmit. Our medical tools do neither of these two things. Our medical tools don't mutate or transmit. We have a fundamental mismatch between our tools, which are static, and the infections, which are dynamic. This mismatch is why we're always flat-footed. This mismatch is why we're playing catch-up. And this mismatch is universal. It's the reason that we have antibiotic-resistant infections that killed 40,000 Americans last year, and it's the reason that the flu vaccine couldn't prevent the flu from killing 60,000 Americans last year. So how do we resolve this fundamental mismatch?
在控制疫情爆发时, 我们所需要面对的根本问题是 病毒和其它传染性疾病 特别擅长的两件事: 它们变异, 而且它们传播。 这是我们的医疗手段无法办到的。 我们的医疗手段 既不会变异也不会传播。 我们需要面对一种根本性的不匹配, 我们的手段是静态的, 而传染是动态的。 这种不匹配也就是为什么 我们总是措手不及, 也就是为什么我们正拼命追赶。 同时这种不匹配是普遍存在的。 这也是为什么去年有 4 万美国人 死于抗生素耐药性感染。 也就是为什么去年流感疫苗 没能防止 6 万美国人死于流感。 那么我们该如何解决 这种根本性的不匹配呢?
I've devoted my career to studying and solving this problem. For 100 years, we've used chemicals as drugs to treat infections. Chemicals will never mutate or transmit. Similarly, our vaccines are not designed to mutate or transmit. 20 years ago, I had a radical idea to use the viruses themselves as therapies -- as building blocks for therapies. To build therapies that could mutate and transmit. Let me share with you how we've had a major breakthrough, and we're already testing these new therapies.
我的职业生涯一直致力于 研究和解决这个问题。 在过去 100 年, 我们利用化学制品作为药品 来治疗传染。 化学制品无法变异或传播。 同理,我们的疫苗设计并不是 为了变异或传播。 20 年前, 我产生了一个激进的想法, 我想利用这些病毒本身 作为治疗手段—— 作为疗法的构成基石, 来构建能够变异和传播的疗法。 我来跟大家分享一下 我们目前取得的重大突破。 我们已经在测试这些新疗法。
HIV is the most devastating pandemic of our era. 75 million infected; 33 million dead. Most of us think that HIV is a solved problem. We have truly amazing antiviral drugs: they're safe and effective, and we've spent 15 years and billions of dollars deploying these drugs around the world. So let's look at the numbers.
艾滋病毒是我们这个时代 最令人闻风丧胆的传染病。 7500 万感染者; 死亡人数达 3300 万。 我们大部分人认为 艾滋病问题已被解决。 我们的确有非常棒的抗病毒药品: 安全且有效, 我们花了 15 年的时间, 花了数十亿美元, 把这些药品运送到了世界各地。 现在我们来看一组数据。
In 2019, 1.7 million people acquired HIV. This number only hit home for me last year when I visited this rural village outside of Durban, South Africa. I was driving along this dirt road with my 10-year-old daughter in the back seat, and walking next to us on the side of the road were girls, the same age as my daughter, barefoot. My daughter asked about why these girls are barefoot and I had to explain disparity to her, which was hard. But what really shocked me was when my colleagues, the local African scientists explained to me that these young girls the same age as my daughter --
在 2019 年, 170 万人感染了艾滋病。 当去年我访问南非德班外 一个偏远的农村时, 我才对这个数字有了深切的感受。 我在一条泥路上开着车, 10 岁的女儿坐在后座, 和我女儿年纪差不多的女孩们, 光脚走在车外。 女儿问我为什么这些女孩子赤着脚, 我得跟她解释什么是贫富差距, 这是很艰深的话题。 但令我震惊的是 我的同事, 当地的非洲科学家跟我解释道, 这些跟我女儿同龄的小女孩——
(Breathes)
(呼吸)
sorry -- had an 80 percent chance of acquiring HIV in their lifetime. It blew me away. How can these girls have an 80 percent risk if we have safe and effective drugs?
抱歉—— 在她们一生中, 罹患艾滋病的风险高达 80% 。 这使我惊呆了。 如果我们有安全有效的药品, 这些女孩子 怎么还会有 80% 的风险?
The reason is the fundamental mismatch. It creates barriers to controlling infectious disease, particularly in resource-limited settings. The first barrier is mutation: viruses mutate, our drugs don't. The second barrier: adherence. It's really hard to get these drugs to those who need the most. I can't even adhere to a week-long antibiotic regimen in this country. We're asking those in resource-limited settings who face enormous adversity to adhere to lifelong regimens.
原因还是根本性的不匹配。 它对传染病防控行程阻碍, 尤其是在资源有限的地区。 第一道阻碍是变异: 病毒会变异,但是我们的药品不会。 第二道阻碍是:对医疗的遵守。 要想把这些药物送到 最急需的人群当中 是十分困难的。 居住在美国的我连服用一周抗生素 这样简单的事都不能遵守。 可我们让那些生活在 资源有限的环境里, 经受着重重苦难的人, 坚持终生治疗。
And the third barrier is deployment, or access. It's super hard to get these drugs to those who need them most. Not these girls but those who engage in high-risk activities, such as commercial sex work and injection drug use. In the epidemiological parlance, these groups are called "super-spreaders." And in the 1900s, a small subset of super-spreaders drove HIV along the Trans-Africa Highway and spread the virus through the continent like this. These groups are exceptionally hard to identify, they're small, they face enormous social stigma so they don't self-identify and they're the ones we need to get to the most. All of these barriers combined created the situation we have today, where greater than 15 percent of people in Southern Africa live with HIV.
第三道阻碍是药物投入, 或获得。 要把这些药物送到最急需的人当中 实在太困难了。 不单单是这些女孩子, 还有那些从事高风险活动的人, 比如说性工作者或使用毒品的人。 用流行病学术语来说, 这些人群被称为“超级传染者”。 在 20 世纪, 一小群超级传染者 携带着艾滋病毒横穿非洲高速公路, 将病毒传染至这整个非洲。 这些人群极难识别, 他们人数不多, 且都顶着莫大的社会污名, 以至于他们也不会自报家门, 他们正是我们最需要触达的人群。 这些阻碍一起造成了 我们今天面临的局面, 也就是非洲南部有超过 15% 的人 携带着艾滋病毒。
Now, conventional wisdom is: what we need to do is get more drugs to more people more effectively. I'd argue we need to solve the fundamental mismatch; we need to eliminate these barriers. If we can build therapies that mutate and transmit, we can overcome drug resistance, overcome adherence barriers, and if we do it properly, we will convert the super-spreaders from the greatest barrier to the most powerful deployment strategy that we can imagine.
传统的智慧告诉我们: 我们需要做的是有效地 给更多的人带来更多的药物。 但是我会提出我们需要解决 根本性的不匹配; 我们需要消除这些阻碍。 如果我们能发明 可以变异和传播的疗法, 我们可以攻克抗药性问题, 解决难以坚持治疗的阻碍, 如果我们采取适当的方法, 我们能将这些超级传染者 从最大的阻碍 转变为我们能想象得到的 最有效的药物投入策略。
This is a radical concept. It has huge potential payoff, but there's a catch. And it's serious. Before we deploy a therapy that may transmit, even if it's only in a limited population of already infected individuals, before we do this, we need to be exceptionally careful, and we need to test safety in the most rigorous ways possible. The reason I'm here today is because for the first time 20 years, we got it to work, and this is the first time I'm sharing it publicly.
这是一个激进的概念。 潜在收益是巨大的, 但是同时有个潜在风险。 非常严重的潜在风险。 在我们部署可以传播的疗法之前, 哪怕只是在 有限的已感染人口中实施, 在我们实施之前, 我们需要异常地小心, 我们需要尽可能用最严谨的方法 测试药物安全性。 今天我站在这里的原因 是因为 20 年来第一次, 我们做到了, 这是我第一次向公众分享。
(Applause and cheers)
(掌声与欢呼)
Last two times I did this I cried, so --
前两次我在分享的时候哭了, 所以——
(Laughter)
(笑声)
So in order to help you understand this breakthrough, let me take you back 20 years to 1999. I was a graduate student in Berkeley, California, studying the biophysics of HIV. For such a complex epidemic, the simplicity of this virus fascinated me. HIV, like all viruses, is just an instruction set -- malware. It hijacks a cell and converts that cell into a factory to do one thing: single-mindedly churn out more virus. All the normal functions of the cell get wiped away. HIV infects the white blood cell that keeps us healthy. This cell has already been hijacked and converted into a factory. And if we magnify, we can see the anatomy of the virus. Those squiggly red lines in the middle? That's HIV's instruction set. Its genetic material.
为了帮助你们更好地了解这项突破, 让我带你们回到 20 年前的 1999年 。 当时的我是 加州伯克利大学的研究生, 正在做艾滋病毒的 生物物理学研究。 对于如此复杂的传染病而言, 这个病毒的简单性让我很着迷。 艾滋病毒就跟所有病毒一样, 只是一个指令集—— 就像病毒软件一样的指令集。 病毒挟持了一个细胞并将它转变成 一个工厂,只干一件事: 一心一意地生产更多的病毒。 这个细胞的其他正常功能 被抹得一干二净。 艾滋病毒感染了 让我们保持健康的白血细胞。 这个细胞已被劫持了, 并被转变成一个工厂。 我们放大来看, 我们可以看到这个病毒的剖面。 能看到中间的 那些弯弯曲曲的红线吗? 那就是艾滋病毒的指令集。 它是基因物质。
This genetic material directs the hijacking process, converting that cell into a factory first to make more copies of the instruction set, and then all the other components of the virus and assemble them into a particle. This is how the virus replicates. Each of these particles can go in and hijack a new cell. This is how the virus transmits. And every time a cell is hijacked, little mistakes are made in copying the genetic material. That's how the virus mutates. This ability to replicate, transmit and mutate is something that our current drugs cannot do.
这个基因物质指挥了劫持的过程, 先将细胞转变成工厂 来制造更多的指令集副本, 再生产这个病毒的所有其他成分。 再将他们组合成一个粒子。 这就是病毒复制的原理。 这里粒子当中的每一个 都可以侵入并劫持一个新的细胞。 这就是病毒传播的原理。 每当一个细胞被劫持, 在复制基因物质的时候, 都会出现一些小错误。 这就是病毒变异的原理。 这种复制、传播和变异的能力 是我们目前的药物无法办到的。
So, being young and naïve and a little bit ignorant, I thought: why can't we create therapies that mutate and transmit and replicate? Here was the idea. If we can take the virus and engineer it to amputate the genetic material in blue here, this amputated instruction set can no longer hijack a cell. But this amputated instruction set can do something very special. In an already infected cell, this amputated instruction set can hijack the hijacker. It can commandeer HIV's machinery to make more copies of itself, the amputated instruction set, and then each of these copies can steal all of HIV's other components so that the cell gets converted from a factory that produces virus to a factory that produces therapy. Hijackers. These carry no disease. This dramatically lowers HIV levels and keeps the cell healthier.
当时年轻,天真又带点儿自负的我, 有个想法: 为什么我们不能创造 可以变异、传播和复制的疗法呢? 这就是我当时的想法。 如果我们能用这个病毒 进行生物工程改造, 来切断蓝色部分的基因物质, 这段被截开的指令集 将不能再劫持细胞。 但是同时它能做一些很特别的事情。 在一个已经被感染的细胞里, 这个被截的指令集可以劫持劫持者。 它可以指令艾滋病毒的机器 复制自己本身, 被截的指令集, 以及它的每一个副本都可以盗取 艾滋病毒的所有其他部分, 如此一来,这个细胞 从一个生产病毒的工厂, 转变为一个生产疗法的工厂。 劫持者, 已经不再携带疾病。 这个方法大幅降低了艾滋病毒水平, 让细胞变得更健康。
This idea consumed me for months. It was the most intense intellectual experience of my life. On every bike ride to lab, on every walk to the coffee shop, on every run in the hills above campus, the ideas, the arguments, the counterarguments, they all came so rapidly in my head, in my inner monologue, that I was physically out of breath. I thought if we can create a therapy that replicates, it would only need to be taken once. It could mutate along with the virus and possibly it could transmit between infected individuals to treat them. It was a therapy that could do all of the things that the virus could do. It solved the fundamental mismatch.
我琢磨这个想法好几个月, 那是我生命中 求知探索最强烈的体验。 骑车去实验室的路上, 走去咖啡厅的路上, 在校园里爬上山丘的路上, 这些想法,这些命题, 这些反命题, 蜂拥而至我的脑海里, 我的内心独白中, 我几乎无法呼吸。 我想着如果我们能创造 一个能复制的疗法, 只需要治疗一次, 就能跟着病毒变异, 还可以在受感染的个体中传播, 去治疗它们。 这是一个如病毒一般的疗法。 它能解决根本性的不匹配。
The most radical part of this concept was that the super-spreaders would also be converted from transmitting the virus to now transmitting the therapy. It was a therapy that would go viral along with the virus. This scared some people. But there's already a precedent: we already inadvertently use therapies that transmit. The vaccine that eradicated polio in the US, the oral polio vaccine, transmits between people. It's not well-known, but the fact that this vaccine transmits is part of the reason that it was chosen for the worldwide eradication effort despite its safety issues.
这个概念最激进的部分是 超级感染者也会 从传播病毒的人 转变为传播治疗方法的人。 这是一个会随着病毒疯传的疗法。 这个想法吓坏了一部分人。 但是已经有了一个先例: 我们已经不经意地 用了这个会传播的疗法。 在美国消灭了小儿麻痹症的疫苗, 口服的小儿麻痹症疫苗, 在人们之间传播。 这并不是街知巷闻的消息, 但是这个疫苗具备传播能力的事实 就是它为什么能被选择 进入全球消灭行动的原因, 尽管有安全问题的担忧。
So the bigger problem was that these hijacker therapies didn't exist. My Berkeley advisors said to me, "Lovely idea, so sad it will never work," or, "Regulators will never allow it, drop it." But the idea wouldn't drop me.
所以更大的问题是 这样的劫持者疗法并不存在。 我的伯克利导师跟我说, “有趣的想法, 可惜它永远不可能成真,” 或者,“立法者是不可能批准的, 放弃把。“ 但是这个想法没有放弃我。
If it ever worked, it would solve the fundamental mismatch. So we tried for years to build it. We tried every trick in the book and failed over and over again. We -- every time we thought we had a good idea, we'd spend months, sometimes years working on it only to come up empty. We once spent five years building 150,000 versions of a hijacker therapy. Every single one failed. I once asked a really bright student what he hoped to learn from me during his PhD --
如果它真的能成功, 它将会解决这个根本性不匹配问题。 所以我们花了多年时间尝试打造。 我们尝试了书籍里的任何诀窍, 失败了一次又一次。 我们—— 每一次都觉得 自己有一个很好的想法, 花了好几个月的时间 有时候甚至好几年, 最后空手而回。 我们还试过花了五年的时间 对一个劫持者疗法 做出了 15 万种版本。 每一个版本都失败了。 我有一次问我所指导的 一个天赋异禀的博士生, 问他希望从我这里学习到什么——
(Laughter)
(笑声)
And he replied, "How to keep going, how to continue moving forward despite zero evidence that there's anything there."
他回答道, “在没有一线生机的情况下, 如何坚持, 如何继续前行。”
(Laughter)
(笑声)
I wonder if he was trying to tell me something.
我怀疑他是否在尝试跟我说些什么。
(Laughter)
(笑声)
By 2018, things looked bad. There was no evidence that a hijacker therapy could be engineered. In fact, we had evidence that it might be impossible. It was time to face the hard truth. This solution that I'd wanted so badly, this hijacker therapy just didn't exist. For 20 years, I had been chasing a ghost.
到 2018 年的时候, 情况变得很糟糕。 没有任何证据证明 可以构建出一个劫持者疗法。 实际上,我们还有证据 证明它或许不可能存在。 是时候去面对残酷的事实了。 我渴求已久的治疗方案, 劫持者治疗方案并不存在。 20 年来, 我都在追寻一个幽灵。
Then one day, Elizabeth, a postdoc in my lab, came to me with this picture. It doesn't look like much. My wife thinks it looks like a pregnancy test.
突然有一天, 我实验室里的一名博士后生, 伊丽莎白(Elizabeth) 拿着一张照片走到我跟前。 看起来没什么特别之处, 我妻子觉得 它看起来像是怀孕测试结果。
(Laughter)
(笑声)
But this little band down here -- that was the amputated genetic material that we had been looking for for 20 years. The entire time that we had been trying to build it and failing, it had evolved by itself in a flask in the back of the lab.
这下面的小小带状物—— 就是那个我们苦苦追寻 20 年的 被截的基因物质。 我们花了那么长时间, 尝试制造但是失败一次又一次, 可它就在实验室的一个角落 自己演变了。
(Audience) What?
(观众)什么?
(Laughter)
(笑声)
We finally had a foothold. And we used this to build the first hijacker. But we had no evidence that what we built was a therapy.
我们终于有了立足点。 我们用此来制造第一个劫持者。 但是没有证据证明 我们的产物是一个疗法。
The first hurdle that any therapy has to clear is testing in a mouse. It can be risky. In our case, if our mice died, so did our funding, and with it, any hopes of this becoming a therapy, let alone a transformative one. After so many failures, we were all pretty skeptical but we didn't really have an alternative. We had to give it a shot; we had to try.
任何疗法第一个需要克服的难关 就是老鼠试验。 这会有风险。 对于我们来说, 如果我们的老鼠死了, 我们的科研资金也跟着完蛋, 所有疗法研究的希望都随之消失, 更不用说是一个革命性的治疗方案。 在那么多次失败之后, 我们都很怀疑, 但是我们别无选择。 我们必须尝试,放手一搏。
Amazingly, the hijacker therapy worked in a mouse, and it worked exactly as we'd predicted 20 years before. It protected the cells in a mouse from HIV. Here are the cells under a microscope. First, HIV in red infects those cells, and then the hijacker, in blue, can be activated, protects those cells and transmits to other cells. We'd finally built the hijacker after 20 years. Everyone in the lab was elated. For me, this was proof of concept. If we could do it for one virus we could do it for others.
神奇的是,劫持者疗法 在一个老鼠身上奏效, 就如同 20 年前 我们预测的那样。 它保护老鼠的细胞 免受艾滋病毒的感染。 这是显微镜下的细胞。 首先,标红的艾滋病毒 感染了那些细胞, 接着,标蓝的劫持者被激活, 来保护这些细胞, 并传播给其他细胞。 我们终于在 20 年后 创造出劫持者。 实验室里的每个人都兴高采烈。 对我个人而言,这证明了一个概念。 如果我们能在一种病毒上实现, 我们便能在其他病毒上同样做。
To understand how this hijacker might impact HIV levels worldwide, we ran computer simulations. Epidemiological models. And the results were pretty amazing. If we do nothing in the hardest-hit parts of Africa, HIV prevalence will stay between 25 and 30 percent. If we manage to introduce drugs to three-quarters of the population or if we ever get the long-sought-after vaccine, we would reduce those numbers down to 20 percent. But those are best-case scenarios. If HIV evolves resistance or if people change their behaviors, these numbers could go right back up to 30 percent or even beyond. The blue is the hijacker therapy. And we've not found a way, either theoretically or experimentally, that HIV can evolve resistance to the hijacker.
为了理解这个劫持者在世界范围 对艾滋病毒水平的可能影响, 我们做了计算机模拟。 流行病模型。 结果相当令人振奋。 如果我们撒手不理 最严重的非洲地区, 艾滋病毒感染率会停留在 25% 到 30% 之间。 如果我们能成功将药物投入到 四分之三的人口当中, 或者我们能获取梦寐以求的疫苗, 我们可以将这个数字降到 20%。 但是,这些都是最理想的状态。 如果艾滋病毒进化出抗药性, 又或者人们改变了他们的行为, 这个数字可能又回到 30% 的水平 或者甚至更高。 蓝色的就是劫持者疗法。 无论是理论上还是试验中, 我们还没有发现, 艾滋病毒会对劫持者产生抗体。
The reason this hijacker works so well is the super-spreaders. If the hijacker is introduced in one place over here, the super-spreaders can pick it up and transmit it through the population. Imagine if 10 years from now, HIV is no longer a pandemic.
劫持者之所以如此有效是 因为超级传播者。 如果劫持者能被引进与此, 超级传播者就可以携带它 并在人群中传播。 想象十年以后艾滋病不再是传染病。
To get there, we have to start large-scale clinical trials in five years, which means initial human tests next year. The FDA has cleared us to start testing in HIV-positive patients who have a terminal cancer and have less than a year left to live. Volunteering for this trial is their last incredibly generous gift to the world. They're called the "Last Gift cohort." And to test in these altruistic patients next year, we have to finish our preclinical tests this year ... and I think we will.
为了实现这个愿景, 我们必须在五年内开展 大规模的临床测试, 也就意味着明年 进行初期的人体测试。 美国药物监管(FDA) 已经批准我们 在癌症晚期, 剩下不到一年存活时间, 并且同时是艾滋病的患者中做测试。 志愿参加这次测试的病人 将给这个世界带来 最后的价值连城无比慷慨的礼物。 他们被称为“最后的献礼队伍”。 为了明年测试这些心怀他人的病人, 我们必须在这年完成 我们的临床前测试…… 我觉得我们一定可以的。
I still meet colleagues who push back and are stridently opposed to letting us move forward with testing. They say, "What if something goes wrong? You can't unrelease it." They say, "There are ethical issues; people can't consent." Well, oral polio vaccine faced similar ethical and safety concerns. In fact, oral polio vaccine faced such an effective misinformation campaign that most people still don't know that it transmits, that it successfully eradicated polio in many countries or that this vaccine is the basis for new vaccines. When we presented this hijacker therapy idea in Africa last year, the African scientists had a different response. They said, "How can you not test this?" They said it's unethical to not test it. So even though we might fail, I think the stakes are too high not to try. If we do nothing, those girls outside of Durban will acquire HIV, and the next time that there's a new virus that emerges, we'll be in the same vulnerable position that we are today with quarantines that are porous and vaccines that we need to wait months for that may not match.
我还在和那些退缩 而且竭力反对我们 进行测试的同事见面。 他们说,“如果出事了呢? 你再也收不回来了。” 他们说,“还有道德伦理问题; 人们不会同意的。” 其实口服小儿麻痹症疫苗也面临过 相似的道德困境和安全忧患。 实际上,口服小儿麻痹症疫苗 面临如此有效的错误信息宣传, 就是因为人们还不知道它会传播, 它在许多国家消灭了小儿麻痹症。 这个疫苗为新一代疫苗打下基础。 当我们去年在非洲介绍 这个劫持者疗法想法的时候, 非洲的科学者的态度截然不同。 他们说,“你为什么还不做测试?” 他们说不去做测试 就是不道义的行为。 哪怕我们可能会失败, 我想不去尝试的代价太高了。 如果我们什么都不做, 这些在德班外面的女孩子 会受到艾滋病毒感染, 下次如果出现新的病毒, 我们还是陷入跟今天一样 脆弱不堪的境地: 隔离错漏百出, 我们翘首等待几个月 却只等来不匹配的疫苗。
I think it's time for a new approach that's different than the static approaches of the last century. It's time for a new technology that is less reactive and more proactive. I think it's time for treatments that don't just benefit the most affluent among us but also those who face the greatest adversity. I think it's time for a new type of weapon that matches, or that solves the fundamental mismatch. I think it's time for therapies that can go viral.
我想是时候采取 与上个世纪的静态手段 不同的新方法。 是时候尝试一种不那么被动反应、 更积极的新技术。 我想是时候尝试新疗法, 不仅让我们当中富裕的人受益, 而且还可以让那些 面临最大困境的人受益。 我想是时候尝试一个新型武器 能与病毒匹敌, 解决根本性不匹配问题的时刻到了。 我想是时候尝试 “病毒式传播”的疗法。
Thank you very much.
谢谢大家。
(Applause)
(掌声)