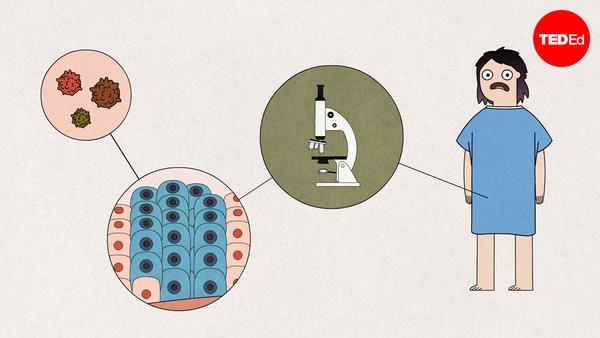
During World War I, one of the horrors of trench warfare was a poisonous yellow cloud called mustard gas. For those unlucky enough to be exposed, it made the air impossible to breathe, burned their eyes, and caused huge blisters on exposed skin.
Tokom Prvog svetskog rata, jedan od užasa rovovskog rata bio je otrovni žuti gas zvani iperit. Kod onih manje srećnih koji su mu bili izloženi izazivao je opstrukciju disanja, iritaciju očiju i velike plikove na nepokrivenim delovima kože.
Scientists tried desperately to develop an antidote to this vicious weapon of war. In the process they discovered the gas was irrevocably damaging the bone marrow of affected soldiers— halting its ability to make blood cells. Despite these awful effects, it gave scientists an idea. Cancer cells share a characteristic with bone marrow: both replicate rapidly. So could one of the atrocities of war become a champion in the fight against cancer? Researchers in the 1930s investigated this idea by injecting compounds derived from mustard gas into the veins of cancer patients. It took time and trial and error to find treatments that did more good than harm, but by the end of World War II, they discovered what became known as the first chemotherapy drugs.
Naučnici su očajnički pokušavali da nađu protivotrov za ovo svirepo ratno oružje. U tom procesu otkrili su da ovaj gas trajno oštećuje koštanu srž zaraženih vojnika, zaustavljajući njenu sposobnost pravljenja krvnih zrnaca. Uprkos ovim užasnim posledicama, naučnici su došli na ideju. Ćelije raka dele zajedničku osobinu sa ćelijama koštane srži: i jedne i druge se brzo repliciraju. Pa su se zapitali da li bi ova ratna grozota mogla postati pobednik u borbi protiv raka? Istraživači su 30-ih godina istraživali ovu ideju tako što su intravenozno ubrizgavali jedinjenja dobijena iz iperita pacijentima koji boluju od raka. Trebalo im je dugo vremena i testiranja da bi pronašli lekove koji proizvode više koristi nego štete, ali pred kraj Drugog svetskog rata, otkrili su prve hemoterapijske lekove.
Today, there are more than 100. Chemotherapy drugs are delivered through pills and injections and use "cytotoxic agents," which means compounds that are toxic to living cells. Essentially, these medicines cause some level of harm to all cells in the body— even healthy ones. But they reserve their most powerful effects for rapidly-dividing cells, which is precisely the hallmark of cancer.
Danas ih ima preko stotinu. Hemoterapijski lekovi se daju putem tableta i injekcija i koriste „citotoksične agense”, tj. jedinjenja toksična za žive ćelije. U suštini, ovi lekovi imaju određene negativne efekte na sve ćelije u telu, čak i na one zdrave. Ali najjači efekti su rezervisani za ćelije koje se brzo dele, što je zaštitni znak kancera.
Take, for example, those first chemotherapy drugs, which are still used today and are called alkylating agents. They’re injected into the bloodstream, which delivers them to cells all over the body. Once inside, when the cell exposes its DNA in order to copy it, they damage the building blocks of DNA’s double helix structure, which can lead to cell death unless the damage is repaired. Because cancer cells multiply rapidly, they take in a high concentration of alkylating agents, and their DNA is frequently exposed and rarely repaired. So they die off more often than most other cells, which have time to fix damaged DNA and don’t accumulate the same concentrations of alkylating agents.
Uzmimo, na primer, prve hemoterapijske lekove, koji se i danas koriste i nazivaju se alkilirajući agensi. Oni se ubrizgavaju u krvotok, i tako dospevaju u ćelije svuda po telu. Dospevši tamo, kad ćelija izloži svoj DNK da bi ga kopirala, oni oštećuju sastavne delove dvostruke spirale DNK, što dovodi do smrti ćelije ukoliko se oštećenje ne popravi. S obzirom na to da se ćelije raka umnožavaju velikom brzinom, one primaju visoku koncentraciju alkilirajućih agenasa i njihova DNK je često izložena, a retko se popravlja. Tako da one izumiru češće nego većina drugih ćelija, koje imaju vremena da poprave oštećenu DNK i ne akumuliraju iste koncentracije alkilirajućih agenasa.
Another form of chemotherapy involves compounds called microtubule stabilizers. Cells have small tubes that assemble to help with cell division and DNA replication, then break back down. When microtubule stabilizers get inside a cell, they keep those tiny tubes from disassembling. That prevents the cell from completing its replication, leading to its death.
Drugi oblik hemoterapije koristi jedinjenja zvana mikrotubularni stabilizatori. Ćelije imaju male cevi koje se sklapaju kako bi pomogle u ćelijskoj deobi i replikaciji DNK, a onda se ponovo razdvajaju. Kad mikrotubularni stabilizatori uđu u ćeliju, oni sprečavaju razdvajanje tih malih cevi.
These are just two examples of the six classes of chemotherapy drugs we use to treat cancer today. But despite its huge benefits, chemotherapy has one big disadvantage: it affects other healthy cells in the body that naturally have to renew rapidly. Hair follicles, the cells of the mouth, the gastrointestinal lining, the reproductive system, and bone marrow are hit nearly as hard as cancer.
Time sprečavaju ćelije da dovrše replikaciju i one izumiru. Ovo su samo dva primera od šest vrsta hemoterapijskih lekova koje danas koristimo u lečenju raka. Uprkos ogromnim pozitivnim efektima, hemoterapija ima jedan veliki nedostatak: ona pogađa druge zdrave ćelije u telu koje prirodno moraju brzo da se obnavljaju. Folikuli kose, ćelije u ustima, gastrointestinalnom epitelu, reproduktivnom sistemu i koštanoj srži pogođene su skoro istom jačinom kao i rak.
Similar to cancer cells, the rapid production of these normal cells means that they’re reaching for resources more frequently— and are therefore more exposed to the effects of chemo drugs. That leads to several common side effects of chemotherapy, including hair loss, fatigue, infertility, nausea, and vomiting. Doctors commonly prescribe options to help manage these side-effects, such as strong anti-nausea medications. For hair loss, devices called cold caps can help lower the temperature around the head and constrict blood vessels, limiting the amount of chemotherapy drugs that reach hair follicles. And once a course of chemo treatment is over, the healthy tissues that’ve been badly affected by the drug will recover and begin to renew as usual.
Slično ćelijama raka, brza proizvodnja ovih normalnih ćelija podrazumeva da one ćešće posežu za resursima i prema tome su izloženije efektima hemoterapijskih lekova. To dovodi do nekoliko nuspojava hemoterapije, kao što su gubitak kose, umor, sterilitet, mučnina i povraćanje. Lekari obično prepisuju opcije za olakšavanje ovih nuspojava, kao što su jaki lekovi protiv mučnine. Za opadanje kose, „hladne kape” mogu sniziti temperaturu na glavi i suziti krvne sudove, smanjujući pritom dotok hemoterapijskih lekova u folikule kose. A po završetku hemoterapijskog lečenja, zdravo tkivo oštećeno od lekova će se oporaviti i početi da se obnavlja kao i obično.
In 2018 alone, over 17 million people world-wide received a cancer diagnosis. But chemotherapy and other treatments have changed the outlook for so many. Just take the fact that up to 95% of individuals with testicular cancer survive it, thanks to advances in treatment. Even in people with acute myeloid leukemia— an aggressive blood cancer— chemotherapy puts an estimated 60% of patients under 60 into remission following their first phase of treatment.
Samo u 2018, preko 17 miliona ljudi širom sveta je obolelo od raka. Hemoterapija i drugi oblici lečenja mnogima su promenili izglede za oporavak. Uzmimo samo činjenicu da je 95% osoba sa rakom testisa preživelo, zahvaljujući napretku u načinima lečenja. Čak i kod osoba sa akutnom mijeloidnom leukemijom, agresivnim oblikom raka krvi, hemoterapija uvodi oko 60% pacijenata ispod 60 godina u remisiju posle prve faze lečenja.
Researchers are still developing more precise interventions that only target the intended cancer cells. That’ll help improve survival rates while leaving healthy tissues with reduced harm, making one of the best tools we have in the fight against cancer even better.
Istraživači i dalje pronalaze još preciznije intervencije koje ciljaju samo ćelije raka. To će podići procenat izlečenja pri čemu će zdrava tkiva trpeti manju štetu i učiniti jedno od najboljih raspoloživih sredstava za borbu protiv raka