I'm a pediatrician and an anesthesiologist, so I put children to sleep for a living. (Laughter) And I'm an academic, so I put audiences to sleep for free. (Laughter) But what I actually mostly do is I manage the pain management service at the Packard Children's Hospital up at Stanford in Palo Alto. And it's from the experience from about 20 or 25 years of doing that that I want to bring to you the message this morning, that pain is a disease.
Son pediatra e anestesista, polo que gaño a vida durmindo nenos. (Risas) Tamén son académico, polo que durmo ao público de balde. (Risas) Pero en realidade dedícome a levar a Unidade de Dor no Hospital Infantil Packard en Stanford, Palo Alto. E coa experiencia de 20 ou 25 anos traballando nisto tráiovos unha mensaxe esta mañá: a dor é unha enfermidade.
Now most of the time, you think of pain as a symptom of a disease, and that's true most of the time. It's the symptom of a tumor or an infection or an inflammation or an operation. But about 10 percent of the time, after the patient has recovered from one of those events, pain persists. It persists for months and oftentimes for years, and when that happens, it is its own disease. And before I tell you about how it is that we think that happens and what we can do about it, I want to show you how it feels for my patients. So imagine, if you will, that I'm stroking your arm with this feather, as I'm stroking my arm right now. Now, I want you to imagine that I'm stroking it with this. Please keep your seat. (Laughter) A very different feeling. Now what does it have to do with chronic pain? Imagine, if you will, these two ideas together. Imagine what your life would be like if I were to stroke it with this feather, but your brain was telling you that this is what you are feeling -- and that is the experience of my patients with chronic pain. In fact, imagine something even worse. Imagine I were to stroke your child's arm with this feather, and their brain [was] telling them that they were feeling this hot torch.
Xeralmente, pénsase na dor coma no síntoma dunha patoloxía e isto é certo a maioría das veces. É o síntoma dun tumor, dunha infección, dunha inflamación ou dunha cirurxía. Pero en arredor do 10% dos casos, os pacientes seguirán padecendo dor despois de recuperarse da enfermidade. Pode persistir meses, e, ás veces, anos. Cando sucede isto, a dor é unha enfermidade por si mesma. Antes de que vos conte como cremos que sucede isto, e qué podemos facer ó respecto, quixera mostrarvos como senten a dor os meus pacientes. Imaxinade, se podedes, que vos acaricio o brazo con esta pluma, como estou acariciando o meu neste intre. Agora quero que imaxinedes que o estou acariciando con isto. Por favor, ficade nos asentos. (Risas) Unha sensación moi diferente. Pero, que ten que ver isto coa dor crónica? Imaxinade, se queredes, as dúas ideas xuntas. Imaxinade como sería a vosa vida se vos acariciasen con esta pluma, pero os vosos cerebros vos din que o que están sentindo é isto: esta é a experiencia dos meus pacientes con dor crónica. De feito, imaxinade algo aínda peor. Imaxinade que estou acariciando o brazo dun fillo voso con esta pluma e o seu cerebro dille que o que sente é esta chama.
That was the experience of my patient, Chandler, whom you see in the photograph. As you can see, she's a beautiful, young woman. She was 16 years old last year when I met her, and she aspired to be a professional dancer. And during the course of one of her dance rehearsals, she fell on her outstretched arm and sprained her wrist. Now you would probably imagine, as she did, that a wrist sprain is a trivial event in a person's life. Wrap it in an ACE bandage, take some ibuprofen for a week or two, and that's the end of the story. But in Chandler's case, that was the beginning of the story. This is what her arm looked like when she came to my clinic about three months after her sprain. You can see that the arm is discolored, purplish in color. It was cadaverically cold to the touch. The muscles were frozen, paralyzed -- dystonic is how we refer to that. The pain had spread from her wrist to her hands, to her fingertips, from her wrist up to her elbow, almost all the way to her shoulder.
Esta era a vivencia de Chandler, unha paciente miña á que vedes na foto. Como podedes ver, é unha rapaza fermosa. Tiña 16 anos cando a coñecín o ano pasado, E quería ser bailarina profesional. Durante un dos seus ensaios de baile, caeu co brazo estendido e torceu o pulso. Probablemente pensedes, igual ca fixo ela, que una torcedura de pulso é trivial na vida dunha persoa. Envólvese cunha venda elástica, Tómase ibuprofeno 1 ou 2 semanas e fin da historia. Pero no caso de Chandler, este foi o inicio da historia. Esta era a pinta do seu brazo cando veu á clínica tres meses despois da torcedura. Fixádevos que o brazo ten a cor alterada, como denegrida. Estaba frío coma o dun cadáver. Os músculos estaban xeados, paralizados --como nós dicimos, distónicos. A dor estendérase dende o pulso cara á man e as puntas dos dedos, e cara ó cóbado. chegando case ó ombreiro.
But the worst part was, not the spontaneous pain that was there 24 hours a day. The worst part was that she had allodynia, the medical term for the phenomenon that I just illustrated with the feather and with the torch. The lightest touch of her arm -- the touch of a hand, the touch even of a sleeve, of a garment, as she put it on -- caused excruciating, burning pain.
Pero o peor non era a dor espontánea que sentía as 24 horas do día. O peor era a alodinia, un termo médico usado para o fenómeno que antes expliquei coa pluma e a chama. O máis leve contacto no brazo --o rozamento dunha man, mesmo o contacto dunha manga, dunha prenda ao poñela-- causáballe unha dor insoportable, moi ardente.
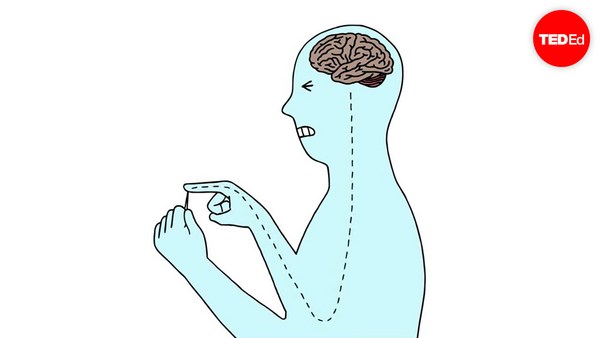
How can the nervous system get this so wrong? How can the nervous system misinterpret an innocent sensation like the touch of a hand and turn it into the malevolent sensation of the touch of the flame? Well you probably imagine that the nervous system in the body is hardwired like your house. In your house, wires run in the wall, from the light switch to a junction box in the ceiling and from the junction box to the light bulb. And when you turn the switch on, the light goes on. And when you turn the switch off, the light goes off. So people imagine the nervous system is just like that. If you hit your thumb with a hammer, these wires in your arm -- that, of course, we call nerves -- transmit the information into the junction box in the spinal cord where new wires, new nerves, take the information up to the brain where you become consciously aware that your thumb is now hurt.
Como pode o sistema nervioso equivocarse dese xeito? Como pode o sistema nervioso confundir una sensación inocente como o tacto dunha man e convertela nunha sensación tan maligna como o contacto cunha chama? Ben, se cadra pensades que o sistema nervioso é como a cablaxe da vosa casa. Nela os cables pasan polas paredes dende o interruptor da luz, a unha caixa de conexións no teito e dende aí ata a lámpada. Cando se calca no interruptor, acéndese a luz. E cando se pecha, a luz apágase. A xente imaxina que o sistema nervioso funciona así. Se pegas cun martelo no polgar, estes cables do brazo --chamados nervios-- transmiten a información á caixa de conexións na medula espiñal onde novos cables, novos nervios, levan a información ata o cerebro, que é cando te das conta de que magoaches o polgar.
But the situation, of course, in the human body is far more complicated than that. Instead of it being the case that that junction box in the spinal cord is just simple where one nerve connects with the next nerve by releasing these little brown packets of chemical information called neurotransmitters in a linear one-on-one fashion, in fact, what happens is the neurotransmitters spill out in three dimensions -- laterally, vertically, up and down in the spinal cord -- and they start interacting with other adjacent cells. These cells, called glial cells, were once thought to be unimportant structural elements of the spinal cord that did nothing more than hold all the important things together, like the nerves. But it turns out the glial cells have a vital role in the modulation, amplification and, in the case of pain, the distortion of sensory experiences. These glial cells become activated. Their DNA starts to synthesize new proteins, which spill out and interact with adjacent nerves, and they start releasing their neurotransmitters, and those neurotransmitters spill out and activate adjacent glial cells, and so on and so forth, until what we have is a positive feedback loop.
Por suposto, a situación no corpo humano é moito máis complexa. Poderíase pensar que a caixa de conexións na medula espiñal é só onde un nervio conecta co seguinte liberando paquetiños marróns de información química que chamamos neurotransmisores de forma linear un a un; pero en realidade o que sucede é que se esparexen en tres dimensións --lateralmente, verticalmente, arriba e abaixo na medula espiñal-- e comezan a interactuar con outras células adxacentes. Estas células, chamadas gliais, antes pensábase que eran elementos estruturais pouco importantes da medula espiñal que non tiñan máis función ca a de unir os elementos importantes, como os nervios. Pero a verdade é que a glía xoga un papel vital na modulación, amplificación e, no caso da dor, na distorsión das experiencias sensoriais. Estas células gliais actívanse. O seu ADN sintetiza novas proteínas que se liberan e interactúan cos nervios adxacentes, e comezan a liberar os seus neurotransmisores. E estes esparéxense, activan células gliais adxacentes, e así sucesivamente, ata que se produza unha retroalimentación positiva.
It's almost as if somebody came into your home and rewired your walls so that the next time you turned on the light switch, the toilet flushed three doors down, or your dishwasher went on, or your computer monitor turned off. That's crazy, but that's, in fact, what happens with chronic pain. And that's why pain becomes its own disease. The nervous system has plasticity. It changes, and it morphs in response to stimuli.
É case como se alguén fora á vosa casa e cambiara a cablaxe das paredes, de modo que a seguinte vez que acendedes a luz funcionara a cadea do WC tres portas máis alá, ou o lavalouza acendera só ou se apagara o monitor do ordenador. É unha loucura, pero de feito, iso é o que sucede coa dor crónica. E por iso a dor convértese nunha enfermidade por si mesma. O sistema nervioso ten plasticidade. Cambia e transfórmase en resposta ós estímulos.
Well, what do we do about that? What can we do in a case like Chandler's? We treat these patients in a rather crude fashion at this point in time. We treat them with symptom-modifying drugs -- painkillers -- which are, frankly, not very effective for this kind of pain. We take nerves that are noisy and active that should be quiet, and we put them to sleep with local anesthetics. And most importantly, what we do is we use a rigorous, and often uncomfortable, process of physical therapy and occupational therapy to retrain the nerves in the nervous system to respond normally to the activities and sensory experiences that are part of everyday life. And we support all of that with an intensive psychotherapy program to address the despondency, despair and depression that always accompanies severe, chronic pain.
E que facemos ó respecto? Que podemos facer nun caso como o de Chandler? Hoxe en día tratamos eses pacientes de forma bastante rudimentaria. Tratámolos con fármacos modificadores dos síntomas --analxésicos-- que verdadeiramente non son moi eficaces para este tipo de dor. Collemos nervios que son ruidosos e activos que deberían estar en silencio, e adormecémolos con analxésicos locais. E o máis importante que facemos é usar un rigoroso, e a miúdo incómodo proceso de terapia física e terapia ocupacional co fin de reeducar os nervios no sistema nervioso para que teñan unha resposta normal ás actividades e experiencias sensoriais que forman parte da vida cotiá. E apoiamos todo isto cun programa de psicoterapia intensiva para enfrontar o desánimo, a desesperación e a depresión que acompañan sempre á dor crónica severa.
It's successful, as you can see from this video of Chandler, who, two months after we first met her, is now doings a back flip. And I had lunch with her yesterday because she's a college student studying dance at Long Beach here, and she's doing absolutely fantastic.
É exitoso, como se pode ver neste vídeo de Chandler quen, dous meses despois de coñecela, está facendo unha viravolta para atrás. Onte comín con ela, porque é unha estudante universitaria de danza en Long Beach, todo lle está indo moi ben.
But the future is actually even brighter. The future holds the promise that new drugs will be developed that are not symptom-modifying drugs that simply mask the problem, as we have now, but that will be disease-modifying drugs that will actually go right to the root of the problem and attack those glial cells, or those pernicious proteins that the glial cells elaborate, that spill over and cause this central nervous system wind-up, or plasticity, that so is capable of distorting and amplifying the sensory experience that we call pain. So I have hope
Pero o futuro é incluso máis brillante. O futuro promete que os novos medicamentos que se desenvolverán non serán fármacos modificadores da sintomatoloxía que simplemente agachan o problema, como facemos agora, senón que serán fármacos modificadores da enfermidade que realmente actuarán na raíz do problema e atacarán ás células gliais ou a esas proteínas prexudiciais que as células gliais elaboran, esparexéndose e provocando no sistema nervioso a sensibilización ou plasticidade, que é capaz de distorsionar e amplificar a experiencia sensorial coñecida como dor. Así, esperamos
that in the future, the prophetic words of George Carlin will be realized, who said, "My philosophy: No pain, no pain."
que no futuro se cumpran as palabras proféticas de George Carlin que dicía: "A miña filosofía: non hai dor, non hai dor"
Thank you very much.
(Risas)
(Applause)
Moitas grazas.