I'd like to tell you about a patient named Donna. In this photograph, Donna was in her mid-70s, a vigorous, healthy woman, the matriarch of a large clan. She had a family history of heart disease, however, and one day, she had the sudden onset of crushing chest pain. Now unfortunately, rather than seeking medical attention, Donna took to her bed for about 12 hours until the pain passed. The next time she went to see her physician, he performed an electrocardiogram, and this showed that she'd had a large heart attack, or a "myocardial infarction" in medical parlance.
Gustaríame falarvos dunha paciente chamada Donna. Nesta fotografía Donna tiña uns 70 anos. Era unha muller vigorosa e sa, a matriarca dunha gran familia. Porén, tiña antecedentes familiares de cardiopatía e, un día, tivo unha dor repentina e opresiva no peito. Desgraciadamente, en lugar de buscar atención médica, Donna deitouse durante 12 horas ata que a dor cesou. A próxima vez que foi ver o seu médico, este fíxolle un electrocardiograma, que mostrou que padecera un grave ataque ao corazón, ou “infarto de miocardio”, falando en termos médicos.
After this heart attack, Donna was never quite the same. Her energy levels progressively waned, she couldn't do a lot of the physical activities she'd previously enjoyed. It got to the point where she couldn't keep up with her grandkids, and it was even too much work to go out to the end of the driveway to pick up the mail. One day, her granddaughter came by to walk the dog, and she found her grandmother dead in the chair. Doctors said it was a cardiac arrhythmia that was secondary to heart failure. But the last thing that I should tell you is that Donna was not just an ordinary patient. Donna was my mother.
Logo dese ataque ao corazón, Donna nunca foi a mesma. A súa enerxía diminuíu progresivamente; xa non podía realizar actividades físicas das que antes gozaba. Chegou a un punto onde non podía xogar cos seus netos e se volveu aínda máis complicado saír á rúa a coller o correo. Un día, a súa neta veu para pasear o can e atopou a súa avoa falecida na cadeira. Os doutores diagnosticaron unha arritmia derivada do fallo cardíaco. A última cousa que debería contarvos é que Donna non foi só unha paciente. Donna era a miña nai.
Stories like ours are, unfortunately, far too common. Heart disease is the number one killer in the entire world. In the United States, it's the most common reason patients are admitted to the hospital, and it's our number one health care expense. We spend over a 100 billion dollars -- billion with a "B" -- in this country every year on the treatment of heart disease. Just for reference, that's more than twice the annual budget of the state of Washington.
As historias coma esta, desgraciadamente, son moi comúns. As cardiopatías son a primeira causa de morte no mundo. Nos Estados Unidos, son a razón máis común de ingreso nos hospitais e o noso maior gasto en atención médica. Gastamos sobre 100 mil millóns de dólares neste país, cada ano, no tratamento de enfermidades cardíacas. Como referencia, é dúas veces máis que o presuposto anual do estado de Washington.
What makes this disease so deadly? Well, it all starts with the fact that the heart is the least regenerative organ in the human body. Now, a heart attack happens when a blood clot forms in a coronary artery that feeds blood to the wall of the heart. This plugs the blood flow, and the heart muscle is very metabolically active, and so it dies very quickly, within just a few hours of having its blood flow interrupted. Since the heart can't grow back new muscle, it heals by scar formation. This leaves the patient with a deficit in the amount of heart muscle that they have. And in too many people, their illness progresses to the point where the heart can no longer keep up with the body's demand for blood flow. This imbalance between supply and demand is the crux of heart failure.
Que fai tan mortal esta enfermidade? Todo comeza co feito de que o corazón é o órgano menos rexenerativo do corpo humano. Un ataque ao corazón ocorre cando se forma un coágulo de sangue nunha arteria coronaria que leva sangue ao corazón. Isto bloquea o fluxo sanguíneo e como o músculo cardíaco é moi activo metabolicamente, morre moi rápido, unhas poucas horas despois do bloqueo. Dado que o corazón non pode rexenerar músculo, cura formando cicatrices. Isto deixa o paciente cun déficit de músculo cardíaco. En moitas persoas, a enfermidade evoluciona ata o punto en que o corazón non pode facer fronte á demanda de sangue do corpo. Este desequilibrio entre a oferta e a demanda é a base do fallo cardíaco.
So when I talk to people about this problem, I often get a shrug and a statement to the effect of, "Well, you know, Chuck, we've got to die of something."
Cando falo coa xente sobre este problema, a miúdo encollen os ombreiros e fan comentarios do tipo: “Mira, Chuck, de algo hai que morrer.”
(Laughter)
(Risas)
And yeah, but what this also tells me is that we've resigned ourselves to this as the status quo because we have to. Or do we? I think there's a better way, and this better way involves the use of stem cells as medicines.
Si, pero isto tamén me di que aceptamos isto como o statu quo porque non queda outra. Ou si? Penso que hai unha maneira mellor, e esta outra forma inclúe o uso de células nai como medicamentos.
So what, exactly, are stem cells? If you look at them under the microscope, there's not much going on. They're just simple little round cells. But that belies two remarkable attributes. The first is they can divide like crazy. So I can take a single cell, and in a month's time, I can grow this up to billions of cells. The second is they can differentiate or become more specialized, so these simple little round cells can turn into skin, can turn into brain, can turn into kidney and so forth. Now, some tissues in our bodies are chock-full of stem cells. Our bone marrow, for example, cranks out billions of blood cells every day. Other tissues like the heart are quite stable, and as far as we can tell, the heart lacks stem cells entirely. So for the heart, we're going to have to bring stem cells in from the outside, and for this, we turn to the most potent stem cell type, the pluripotent stem cell. Pluripotent stem cells are so named because they can turn into any of the 240-some cell types that make up the human body.
Pero que son exactamente as células nai? Se as vemos a través do microscopio, non hai moito que ver. Son células redondas, pequenas e simples. Pero isto oculta dous atributos notables. O primeiro é que se dividen coma tolas. Podo coller unha única célula e, nun mes, facer que se divida en miles de millóns de células. O segundo é que se poden diferenciar ou chegar a estar máis especializadas, así que estas pequenas células redondas poden converterse en pel, en cerebro, nun ril e demais. Agora ben, algúns tecidos corporais están repletos de células nai. A nosa medula ósea, por exemplo, produce miles de millóns de células cada día. Outros tecidos, coma o corazón, son bastante estables, e polo que podemos saber ata agora, este carece totalmente de células nai. Entón, para o corazón imos ter que traer células nai do exterior, e para isto recorremos ao tipo de célula nai máis potente, a célula nai pluripotente. As células nai pluripotentes denomínanse así porque poden converterse en calquera dos 240 tipos de células que compoñen o corpo humano.
So this is my big idea: I want to take human pluripotent stem cells, grow them up in large numbers, differentiate them into cardiac muscle cells and then take them out of the dish and transplant them into the hearts of patients who have had heart attacks. I think this is going to reseed the wall with new muscle tissue, and this will restore contractile function to the heart.
Esta é a miña gran idea: quero tomar células nai pluripotentes humanas, crialas en grandes cantidades, facer que se convertan en células do músculo cardíaco e logo sacalas do medio de cultivo e transplantalas aos corazóns de persoas que sufriron ataques cardíacos. Penso que isto vai reconstruír a parede con novo tecido muscular e restaurará a función contráctil do corazón.
(Applause)
(Aplausos)
Now, before you applaud too much, this was my idea 20 years ago.
Antes de que aplaudades demasiado, esta foi a miña idea hai 20 anos.
(Laughter)
(Risas)
And I was young, I was full of it, and I thought, five years in the lab, and we'll crank this out, and we'll have this into the clinic. Let me tell you what really happened.
Era novo, estaba cheo de entusiasmo e pensaba: “en cinco anos no laboratorio arranxamos isto e témolo na clínica.” Deixádeme contarvos que ocorreu realmente. (Risas)
(Laughter)
Comezamos coa misión de trocar células nai pluripotentes en músculo cardíaco.
We began with the quest to turn these pluripotent stem cells into heart muscle. And our first experiments worked, sort of. We got these little clumps of beating human heart muscle in the dish, and that was cool, because it said, in principle, this should be able to be done. But when we got around to doing the cell counts, we found that only one out of 1,000 of our stem cells were actually turning into heart muscle. The rest was just a gemisch of brain and skin and cartilage and intestine. So how do you coax a cell that can become anything into becoming just a heart muscle cell?
Os nosos primeiros experimentos funcionaron, ou algo así. Obtivemos pequenos grupos de músculo cardíaco que batía no cultivo, e iso estaba ben porque significaba, en principio, que era posible facelo. Pero cando fixemos o reconto de células, descubrimos que só unha entre 1000 células nai estaba a converterse realmente en músculo cardíaco. As demais eran só unha mestura de células cerebrais, da pel, da cartilaxe e do intestino. Como se convence unha célula que pode converterse en calquera cousa para que torne nunha célula muscular cardíaca?
Well, for this we turned to the world of embryology. For over a century, the embryologists had been pondering the mysteries of heart development. And they had given us what was essentially a Google Map for how to go from a single fertilized egg all the way over to a human cardiovascular system. So we shamelessly absconded all of this information and tried to make human cardiovascular development happen in a dish. It took us about five years, but nowadays, we can get 90 percent of our stem cells to turn into cardiac muscle -- a 900-fold improvement. So this was quite exciting.
Para isto acudimos ao mundo da embrioloxía. Durante máis dun século, os embriólogos pensaron nos misterios do desenvolvemento do corazón e déronnos o que era esencialmente un mapa de Google sobre como pasar dun só óvulo fecundado a todo un sistema cardiovascular humano. Así que usamos descaradamente toda esa información e tratamos de facer que o desenvolvemento cardiovascular ocorrese nun cultivo. Levounos cinco anos, pero, hoxe, logramos que o 90 % das nosas células nai se convertan en músculo cardíaco, unha mellora 900 veces maior. Isto foi bastante emocionante.
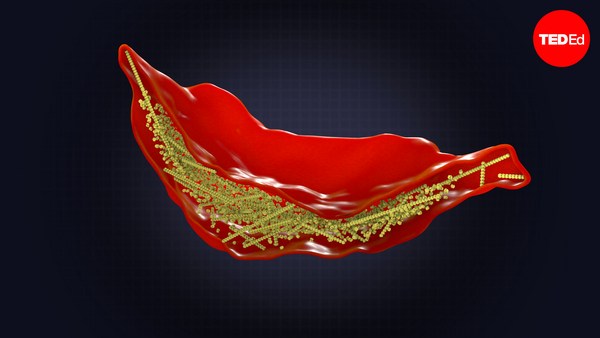
This slide shows you our current cellular product. We grow our heart muscle cells in little three-dimensional clumps called cardiac organoids. Each of them has 500 to 1,000 heart muscle cells in it. If you look closely, you can see these little organoids are actually twitching; each one is beating independently. But they've got another trick up their sleeve. We took a gene from jellyfish that live in the Pacific Northwest, and we used a technique called genome editing to splice this gene into the stem cells. And this makes our heart muscle cells flash green every time they beat.
Esta diapositiva mostra o noso produto celular actual. Facemos crecer as nosas células musculares cardíacas en grupos tridimensionais chamados organoides cardíacos. Cada un deles ten de 500 a 1000 células de músculo cardíaco. Se miramos de cerca, veremos como eses organoides se contraen; cada un latexa de forma independente. Pero teñen outro truco baixo a manga. Collemos un xene dunha medusa que vive no noroeste do Pacífico e empregamos unha técnica chamada edición do xenoma para empalmar este xene nas células nai. Isto fai que as células emitan un brillo verde cada vez que latexan.
OK, so now we were finally ready to begin animal experiments. We took our cardiac muscle cells and we transplanted them into the hearts of rats that had been given experimental heart attacks. A month later, I peered anxiously down through my microscope to see what we had grown, and I saw ... nothing. Everything had died. But we persevered on this, and we came up with a biochemical cocktail that we called our "pro-survival cocktail," and this was enough to allow our cells to survive through the stressful process of transplantation. And now when I looked through the microscope, I could see this fresh, young, human heart muscle growing back in the injured wall of this rat's heart. So this was getting quite exciting.
Ben, agora xa estabamos listos para comezar os experimentos en animais. Collemos as células musculares cardíacas e transplantámolas nos corazóns das ratas que recibiran ataques cardíacos experimentais. Un mes máis tarde, mirei ansioso a través do meu microscopio para ver o que crearamos e vin... nada. Todo morrera. Porén, perseveramos e elaboramos un cóctel bioquímico ao que lle demos o nome de “cóctel prosupervivencia”, que foi suficiente para que as nosas células sobrevivisen ao estresante proceso do transplante. Esta vez, cando mirei polo microscopio, vin un músculo do corazón humano novo e fresco medrar na parede lesionada do corazón da rata. A cousa íase poñendo emocionante.
The next question was: Will this new muscle beat in synchrony with the rest of the heart? So to answer that, we returned to the cells that had that jellyfish gene in them. We used these cells essentially like a space probe that we could launch into a foreign environment and then have that flashing report back to us about their biological activity. What you're seeing here is a zoomed-in view, a black-and-white image of a guinea pig's heart that was injured and then received three grafts of our human cardiac muscle. So you see those sort of diagonally running white lines. Each of those is a needle track that contains a couple of million human cardiac muscle cells in it. And when I start the video, you can see what we saw when we looked through the microscope. Our cells are flashing, and they're flashing in synchrony, back through the walls of the injured heart.
A seguinte pregunta era: latexará este novo músculo en sincronía co resto do corazón? Para responder a isto, volvemos ás células co xene da medusa. Esencialmente, usamos estas células como unha sonda espacial que poderiamos lanzar nun ambiente estraño e nos informaría con eses flashes da súa actividade biolóxica. O que vedes aquí é unha vista ampliada, unha imaxe en branco e negro do corazón dunha cobaia que foi ferida e recibiu tres enxertos do noso músculo cardíaco humano. ¿Vedes esas liñas brancas en diagonal? Cada unha delas é unha marca de agulla que contén un par de millóns de células musculares cardíacas humanas. Cando empece o vídeo, veredes o que observamos cando miramos a través do microscopio. As nosas células brillan, e fano en sincronía, a través das paredes do corazón lesionado.
What does this mean? It means the cells are alive, they're well, they're beating, and they've managed to connect with one another so that they're beating in synchrony. But it gets even more interesting than this. If you look at that tracing that's along the bottom, that's the electrocardiogram from the guinea pig's own heart. And if you line up the flashing with the heartbeat that's shown on the bottom, what you can see is there's a perfect one-to-one correspondence. In other words, the guinea pig's natural pacemaker is calling the shots, and the human heart muscle cells are following in lockstep like good soldiers.
Que significa isto? Quere dicir que as células están vivas, que están ben, que latexan e conseguiron conectarse entre elas para latexar en sincronía. Pero é aínda máis interesante ca isto. Se mirades este trazo da parte inferior, ese é o electrocardiograma do corazón da cobaia. E se aliñades o flash co latexo do corazón que se mostra na parte inferior, veredes unha correspondencia perfecta un a un. Noutras palabras, o marcapasos natural da cobaia leva o mando e as células do músculo cardíaco humano seguen o seu paso seguro coma bos soldados.
(Applause)
(Aplausos)
Our current studies have moved into what I think is going to be the best possible predictor of a human patient, and that's into macaque monkeys. This next slide shows you a microscopic image from the heart of a macaque that was given an experimental heart attack and then treated with a saline injection. This is essentially like a placebo treatment to show the natural history of the disease. The macaque heart muscle is shown in red, and in blue, you see the scar tissue that results from the heart attack. So as you look as this, you can see how there's a big deficiency in the muscle in part of the wall of the heart. And it's not hard to imagine how this heart would have a tough time generating much force.
Os nosos estudos actuais trasladáronse ao que penso que será o mellor indicador posible para un paciente humano: falamos dos macacos. Esta seguinte diapositiva amosa unha imaxe microscópica do corazón dun macaco que recibiu un ataque cardíaco experimental e logo un tratamento de solución salina. Isto é como un tratamento con placebo para amosar o curso natural da enfermidade. O músculo cardíaco do macaco móstrase en vermello e en azul vedes o tecido cicatrizante que resulta do ataque cardíaco. Como vedes, hai unha gran deficiencia no músculo en parte da parede do corazón. Non é difícil de imaxinar o traballo que lle dará a este corazón xerar forza abondo.
Now in contrast, this is one of the stem-cell-treated hearts. Again, you can see the monkey's heart muscle in red, but it's very hard to even see the blue scar tissue, and that's because we've been able to repopulate it with the human heart muscle, and so we've got this nice, plump wall.
En cambio, este é un corazón tratado con células nai. Vemos de novo o músculo cardíaco do mono en vermello, pero é moi difícil ver o tecido azul cicatrizante, e iso é porque puidemos repoboalo co músculo do corazón humano e así obtemos esta parede boa e gordiña.
OK, let's just take a second and recap. I've showed you that we can take our stem cells and differentiate them into cardiac muscle. We've learned how to keep them alive after transplantation, we've showed that they beat in synchrony with the rest of the heart, and we've shown that we can scale them up into an animal that is the best possible predictor of a human's response. You'd think that we hit all the roadblocks that lay in our path, right? Turns out, not.
Ben, recapitulemos un segundo. Mostreivos que podemos tomar as nosas células nai e transformalas en músculo cardíaco. Aprendemos a mantelas vivas logo do transplante, demostramos que latexan en sincronía co resto do corazón e que podemos aumentalas a escala para un animal que é o mellor indicador posible da resposta en humanos. Pensaredes que superamos todos os obstáculos do camiño, non? Pois resulta que non.
These macaque studies also taught us that our human heart muscle cells created a period of electrical instability. They caused ventricular arrhythmias, or irregular heartbeats, for several weeks after we transplanted them. This was quite unexpected, because we hadn't seen this in smaller animals. We've studied it extensively, and it turns out that it results from the fact that our cellular graphs are quite immature, and immature heart muscle cells all act like pacemakers. So what happens is, we put them into the heart, and there starts to be a competition with the heart's natural pacemaker over who gets to call the shots. It would be sort of like if you brought a whole gaggle of teenagers into your orderly household all at once, and they don't want to follow the rules and the rhythms of the way you run things, and it takes a while to rein everybody in and get people working in a coordinated fashion. So our plans at the moment are to make the cells go through this troubled adolescence period while they're still in the dish, and then we'll transplant them in in the post-adolescent phase, where they should be much more orderly and be ready to listen to their marching orders. In the meantime, it turns out we can actually do quite well by treating with anti-arrhythmia drugs as well.
Estes estudos sobre macacos tamén nos ensinaron que as nosas células cardíacas creaban un período de inestabilidade eléctrica. Causaron arritmias ventriculares ou latidos irregulares do corazón durante varias semanas despois de que as transplantásemos. Isto foi bastante inesperado, porque non o viramos en animais máis pequenos. Estudiámolas en detalle e descubrimos que isto ocorre porque os nosos enxertos celulares son bastante inmaturos, e todas as células cardíacas inmaturas actúan como marcapasos. O que pasa é que, ao metelas no corazón, comeza a haber unha competición co marcapasos natural do corazón sobre quen leva a voz cantante. Sería algo así coma se trouxésedes unha manda de adolescentes á vosa casa ordenada, todos á vez, e non quixesen seguir as normas nin os vosos ritmos de facer as cousas. Levaríavos un tempo controlar a todos e conseguir que traballasen de forma coordinada. Polo tanto, os nosos plans neste momento son facer que as células pasen ese convulso período de adolescencia mentres aínda están no cultivo e despois transplantalas na fase postadolescente, cando deberían ser moito máis ordenadas e estar preparadas para obedecer as ordes. Mentres tanto, resulta que nos vai bastante ben tratando con fármacos contra as arritmias.
So one big question still remains, and that is, of course, the whole purpose that we set out to do this: Can we actually restore function to the injured heart? To answer this question, we went to something that's called "left ventricular ejection fraction." Ejection fraction is simply the amount of blood that is squeezed out of the chamber of the heart with each beat. Now, in healthy macaques, like in healthy people, ejection fractions are about 65 percent. After a heart attack, ejection fraction drops down to about 40 percent, so these animals are well on their way to heart failure. In the animals that receive a placebo injection, when we scan them a month later, we see that ejection fraction is unchanged, because the heart, of course, doesn't spontaneously recover. But in every one of the animals that received a graft of human cardiac muscle cells, we see a substantial improvement in cardiac function. This averaged eight points, so from 40 to 48 percent. What I can tell you is that eight points is better than anything that's on the market right now for treating patients with heart attacks. It's better than everything we have put together. So if we could do eight points in the clinic, I think this would be a big deal that would make a large impact on human health.
Aínda queda unha gran pregunta, que é, por suposto, o propósito co que empezamos a facer isto: podemos realmente restaurar a función dun corazón ferido? Para responder a esta cuestión, pasamos a algo chamado “fracción de expulsión ventricular esquerda”. A fracción de expulsión é simplemente a cantidade de sangue que se expulsa fóra da cámara do corazón con cada latexo. En macacos sans, como en persoas sas, as fraccións de expulsión son dun 65 %. Despois dun ataque ao corazón, a fracción de expulsión cae ata un 40 %, polo que estes animais están camiño da insuficiencia cardíaca. Nos animais que reciben unha inxección de placebo, cando os escaneamos un mes despois, vemos que a fracción de expulsión non cambia, porque o corazón, por suposto, non se recupera espontaneamente. Pero en todos os animais que recibiron un enxerto de células do músculo cardíaco humano, observamos unha mellora substancial da función cardíaca, cunha media de oito puntos, do 40 ao 48 %. O que vos podo dicir é que oito puntos é mellor que calquera cousa que haxa no mercado agora mesmo para tratar pacientes con infartos. É mellor que todo o que fixemos ata agora. Se puidésemos facer oito puntos na clínica, sería un grande avance cun enorme impacto na saúde humana.
But it gets more exciting. That was just four weeks after transplantation. If we extend these studies out to three months, we get a full 22-point gain in ejection fraction.
Pero a cousa ponse máis emocionante. Iso foi só catro semanas despois do transplante. Se ampliamos estes estudos a tres meses, obtemos unha mellora de 22 puntos na fracción de expulsión.
(Applause)
(Aplausos)
Function in these treated hearts is so good that if we didn't know up front that these animals had had a heart attack, we would never be able to tell from their functional studies.
A función destes corazóns tratados é tan boa que se non soubésemos de antemán que estes animais sufriran un infarto, nunca seriamos capaces de dicilo a partir dos seus estudos funcionais.
Going forward, our plan is to start phase one, first in human trials here at the University of Washington in 2020 -- two short years from now. Presuming these studies are safe and effective, which I think they're going to be, our plan is to scale this up and ship these cells all around the world for the treatment of patients with heart disease. Given the global burden of this illness, I could easily imagine this treating a million or more patients a year.
No futuro, o noso plan é comezar a fase un, primeiro en ensaios con humanos aquí, na Universidade de Washington, en 2020, dentro de só dous anos. Asumindo que estes estudos sexan seguros e eficaces, e eu penso que o van ser, o noso plan é ampliar isto e enviar estas células a todo o mundo para tratar pacientes con enfermidades cardíacas. Dada a carga global desta enfermidade, poderiamos tratar facilmente un millón de pacientes, ou máis, ao ano.
So I envision a time, maybe a decade from now, where a patient like my mother will have actual treatments that can address the root cause and not just manage her symptoms. This all comes from the fact that stem cells give us the ability to repair the human body from its component parts.
Imaxino un momento, tal vez dentro dunha década, no que un paciente coma a miña nai terá tratamentos que poidan abordar a raíz do problema en lugar de manexar os seus síntomas. Todo isto débese a que as células nai nos dan a capacidade de reparar o corpo humano a partir dos seus compoñentes.
In the not-too-distant future, repairing humans is going to go from something that is far-fetched science fiction into common medical practice. And when this happens, it's going to have a transformational effect that rivals the development of vaccinations and antibiotics.
Nun futuro non moi afastado, reparar humanos vai pasar de ser unha idea tola de ciencia ficción a unha práctica médica común. E cando isto suceda, vai ter un efecto transformador que rivalizará co desenvolvemento das vacinas e antibióticos.
Thank you for your attention.
Grazas pola vosa atención.
(Applause)
(Aplausos)